AbstractPurposeHepatocellular carcinoma (HCC) is one of the most aggressive malignancies. Recently, the overexpression of programmed cell death 1 (PD-1) and PD-1 ligand 1 (PD-L1) has been shown to correlate with poor prognosis in many cancers. However, the expression of PD-L1 or PD-1 ligand 2 (PD-L2) and clinical outcomes have not been fully investigated in HCC.
Materials and MethodsFormalin-fixed paraffin-embedded samples were obtained from 85 patients with HCC who underwent surgery. The expression of PD-Ls (PD-L1, PD-L2) was evaluated by immunohistochemical analysis.
ResultsThe proportion of high expression groups of PD-L1 and PD-L2 was 27.1% and 23.5%, respectively. Univariate analysis revealed that tumor size (p < 0.001), histological differentiation (p=0.010), PD-L1 expression (p < 0.001), and PD-L2 expression (p=0.039) were significant prognostic factors of overall survival in patients with HCC. Multivariate analysis revealed that overall tumor size (hazard ratio [HR], 4.131; 95% confidence interval [CI], 2.233 to 7.643; p < 0.001 and HR, 3.455; 95% CI, 1.967 to 6.067; p < 0.001) and PD-L1 expression (HR, 5.172; 95% CI, 2.661 to 10.054; p < 0.001 and HR, 3.730; 95% CI, 1.453 to 9.574; p=0.006) were independent prognostic values for overall and disease-free survival. Patients with high expression of PD-Ls had a significantly poorer survival than those with low expression (p < 0.001, p=0.034).
IntroductionHepatocellular carcinoma (HCC) is one of the most aggressive malignancies, accounting for over 1 million deaths annually worldwide. There is a clear, causative relationship between HCC and hepatitis B virus (HBV) infection. The highest incidence of disease (> 10 to 20 cases per 100,000) is found in central and Southeast Asia, and in tropical Africa [1]. South Korea is also a high incidence area at 24.5 per 100,000. Moreover, according to the Korean Central Cancer Registry of 2010, HCC is the second and fourth most common cause of cancer death in males and females, respectively, in South Korea. Compounded by underlying cirrhosis, the majority of patients with HCC can be treated with palliative therapy using transarterial chemoembolization or sorafenib [2]. However, sorafenib is limited by its high cost and side effects, which include diarrhea, alopecia, fatigue, cutaneous desquamation, and hypertension. Additionally, sorafenib cannot induce tumor necrosis, although it can inhibit the growth of HCC [3]. After strategies to minimize tumor growth with all of the above therapeutic modalities have failed, only supportive care can be provided. Thus, new therapeutic modalities are needed.
Programmed cell death 1 (PD-1) is an inhibitory receptor of T cells and activated B cells. This receptor is a member of the CD28 family that interacts with the B7 family ligands, including PD-1 ligand 1 (PD-L1, B7-H1) and PD-L2 (B7-DC). These ligands are key check-point molecules of T cells. While PD-L1 is generally expressed on both hematopoietic cells and non-hematopoietic cells, such as T cells, B cells, endothelial cells, and epithelial cells, PD-L2 expression is limited to antigen presenting cells and macro-phages [4]. The interaction of PD-1 and PD-Ls (PD-L1 and PD-L2) is generally correlated with immune tolerance and evasion by tumor cells. The prognostic significance of PD-Ls and the anti-tumor effects of anti–PD-1 antibody have also been reported in many cancers, including breast, lung, ovarian, and melanoma. However, the roles of PD-Ls in antitumor immunity and their clinical significance have not been fully investigated in HCC. Therefore, in the present study, we examined the expression of PD-Ls in different HCC tissues by immunohistochemical staining and investigated the correlation of overexpression of PD-Ls and prognosis in HCC.
Materials and Methods1. Patients and samplesEighty-five patients who underwent macroscopically complete curative resection between January 2001 and January 2010 at Soonchunhyang University Cheonan and Bucheon hospitals with HCC that was pathologically confirmed and formalin-fixed, paraffin-embedded samples were selected. No patients received preoperative chemotherapy or radiotherapy, and none had distant metastasis. No patients died within 30 days of surgery. Patients lost to follow up were not included. All of the clinicopathological data were collected by retrospective review of medical charts and pathological records. The clinicopathological parameters followed the rules for the study of primary HCC, third edition, in June 2007, Korea. Tumor differentiation (grade) was assessed using the Edmondson and Steiner nuclear grading system. Tumor stage was defined according to TNM classification of the American Joint Committee on International Union against Cancer, Okuda staging, Barcelona Clinical Liver Cancer (BCLC) staging and Modified Union for International Cancer Control (UICC) staging. The Institutional Review Board of the Soonchunhyang University Cheonan Hospital approved the study (SCHCA 2015-10-020-002).
2. ImmunohistochemistrySamples were sectioned with a thickness of 4 μm and the antigen was retrieved by heating the slides in antigen retrieval solution (0.01 M citrate buffer, pH 6.0). Peroxidase was inhibited with 3% hydrogen peroxidase in methanol for 40 min at room temperature. Primary antibodies were diluted 1:50 (PD-L1 and PD-L2). The sections were allowed to react with primary antibodies for 2 hours at room temperature, then reacted with a secondary antibody EnVision HRP-Labeled Polymer (Dako, Carpinteria, CA). The slides were then visualized using 3,3′-diaminobenzidine chromogen (Dako), and counterstained with hematoxylin (Muto Pure Chemical Ltd., Tokyo, Japan). Protein expression levels were assessed by two independent pathologists without clinical information using light microscopy.
3. Semiquantitative analysis of PD-LsTwo independent pathologists who were blinded to the clinical outcomes of the patients examined the stained slides. The pathologists determined the expression of PD-Ls semiquantitatively by assessing the percentage of positively stained immunoreactive cells and staining intensity. The staining percentage (0 points, < 10%; 1 point, 10%-50%; and 2 points, > 50%) and intensity of PD-Ls (0, no staining; 1, weak staining; 2, moderate staining; and 3, strong staining) in tumor cells were scored, and the overall score for PD-Ls expression was the sum of the scores. The samples were divided into two groups for statistical analysis according to the overall scores: low expression scores from 0-2 and high-expression scores from 3 to 5. After the initial independent evaluation, both pathologists combined their scores and discussed the results to resolve any disparities.
4. Statistical analysisAll data were analyzed using PASW Statistics ver. 18.0 (SPSS Inc., Chicago, IL) with p < 0.05 as the threshold of statistical significance. Chi-squared and Fisher exact tests were used to compare the levels of PD-Ls expression and various clinicopathological characteristics between the groups. Survival curves for overall survival (OS) and disease-free survival (DFS) were calculated using the Kaplan-Meier method and compared by the log-rank test. Multivariate analysis of prognostic relevance was evaluated by multivariate Cox regression analysis.
Results1. Association between PD-L1 and PD-L2 expression and clinicopathological characteristics of patients with HCCAmong 85 HCC tissue samples, immunohistochemical staining with anti–PD-L1 and anti–PD-L2 antibodies displayed yellow or brown staining in the cell membrane and cytoplasm. The PD-L1 expression level was scored as 0-1, 2, 3-4, and 5 in 22 (25.9%), 40 (47.1%), 18 (21.2%), and five (5.8%) samples, respectively. The PD-L2 expression level was scored as 0-1, 2, 3-4, and 5 in 38 (44.7%), 22 (25.9%), 17 (20.0%), and three (3.5%) samples, respectively. Accordingly, the proportion of high expression groups (scores of 3-5) of PD-L1 and PD-L2 was 27.1% and 23.5%, respectively (Fig. 1). Other clinicopathological characteristics of the PD-Ls are shown in Table 1. PD-L1 expression was strongly correlated with tumor size (p=0.049), recurrence (p=0.028), and PIVKA-II (p=0.037). PD-L2 expression was related to histological differentiation (p=0.002) in patients with HCC. However, no significant correlations were observed between PD-Ls expression and the following clinicopathological variables: age, sex, liver cirrhosis, tumor stage, portal vein invasion, microvascular invasion and α-fetoprotein.
2. Univariate and multivariate survival analysisThe Cox proportional hazard model was used to determine if the independent factors affected the rates of OS and DFS in patients with HCC (Tables 2 and 3). Univariate analyanalysis revealed that tumor size (p < 0.001), histological differentiation (p=0.010), BCLC stage (p=0.033), modified UICC stage (p=0.009), microvascular invasion (p=0.016), PD-L1 expression (p < 0.001), and PD-L2 expression (p=0.039) were significant prognostic factors of OS in patients with HCC. Significant factors for DFS were tumor size (p < 0.001), metastasis (p=0.004), and PD-L1 (p < 0.001) (Table 2). Multivariate analysis showed that tumor size (hazard ratio [HR], 4.131; 95% confidence interval [CI], 2.233 to 7.643; p < 0.001), PD-L1 expression (HR, 5.172; 95% CI, 2.661 to 10.054; p < 0.001), and PD-L2 expression (HR, 1.960; 95% CI, 1.043 to 3.684; p=0.037) were independent prognostic factors of OS. The prognostic factors for DFS were tumor size (HR, 3.835; 95% CI, 2.190 to 6.714; p < 0.001) and PD-L1 expression (HR, 3.730; 95% CI, 1.453 to 9.574; p=0.006) (Table 3).
Kaplan-Meier analysis and the log-rank test demonstrated that the 5-year survival rate of high expression groups of PD-Ls were significantly worse than those of low expression groups (p < 0.001, p=0.034) (Fig. 2A and C). The median survival times in the low PD-L1 and PD-L2 expressing groups were 94 and 67 months, compared with 11 and 22 months for the high PD-L1 and PD-L2 expressing groups, respectively. The recurrence rates were also higher in the high PD-L1 expressing group than in the low PD-L1 expressing group (p < 0.001) (Fig. 2). However, PD-L2 expression was correlated with an impaired DFS, but the difference was not statistically significant (p=0.321). We also investigated combined PD-Ls expression and clinical outcomes, including OS and recurrence. The patients were divided into three groups: I, both low (n=50); II, either high (n=27); and III, both high (n=8). The median OS and DFS were 87 and 31 months for group I, 34 and 12 months for group II, and 6 and 3 months for group III. There were significant differences between each group for OS (I vs. II, p=0.007; I vs. III, p < 0.001; II vs. III, p=0.009), and significant differences in recurrence were also found between groups I and III (p < 0.001), and groups II and III (p=0.007). However, disease free survival for groups I and II did not reach significance.
DiscussionMany studies have reported that PD-1 inhibits T-cells proliferation, survival and function in in vitro and in vivo. Some studies of chronic inflammation and autoimmune disease have shown that PD-1 lymphocyte levels tend to be elevated in many autoimmune diseases, such as rheumatoid arthritis and Sjogren’s syndrome. Moreover, antiviral effects have been reported in chronic lymphocytic choriomeningitis infection and human immunodeficiency virus infection [5]. In malignancies, several studies have demonstrated that PD-L1 was associated with poor prognosis in other cancers, including melanoma, non-small cell lung carcinoma, esophageal carcinoma, gastric carcinoma, pancreatic carcinoma, renal cell carcinoma, and ovarian carcinoma [4,6-11].
In the present study, PD-L1 and PD-L2 were overexpressed in up to 27.1% and 23.5% of HCC specimens. These rates were not higher than those found for other malignancies, including cancers of the lung (50%), esophagus (44%), stomach (42%), breast (23%), and kidney (37%) [12]. We did find that PD-L1 was significantly correlated with tumor size, recurrence and PIVKA-II levels, and that PD-L2 levels were correlated with histological differentiation. Moreover, we found that patients with low expression of PD-Ls had significantly better survival than those with high expression in each group. In particular, simultaneous overexpression of both PD-Ls was more strongly correlated with poorer survival and postoperative recurrence compared to low expression of both PD-Ls. Multivariate analyses supported the finding that the expression of PD-Ls and tumor size were significantly associated with poorer prognosis independent of other potentially confounding factors, such as histological differentiation, presence of microvascular invasion, and tumor stage, which was also examined in univariate analyses. Although the overexpression of PD-L2 was not related to the postoperative recurrences in multivariate analyses, other factors, including overexpression of PD-L1 and tumor size were significantly associated with tumor recurrences. These results were similar to those of a previous study by Gao et al. [13]. Although the proportion of cirrhosis and HBV positive were higher when compared with our study (88% vs. 99.4%), their study also revealed a relationship between PD-L2 and clinical prognosis. These investigators not only looked into PD-Ls expression, but also granzyme B+, FoxP3+ regulatory T-cells infiltration on tissue microarrays of 240 patients with HCC. They reported that overexpression of PD-L2 and PD-L1 were significantly related to poorer survival, but that the difference in recurrence was not statistically significant [13]. These findings indicate that HBV infection had less of an effect on PD-L1 and PD-L2 expression levels in HCC, and that PD-1 blockade is more important than single PD-L1 or PD-L2 knockdown in targeting cancer. Another study that lacked clinical or prognostic data also showed that the expression of PD-L1 in HBV and HCC patients was higher at earlier stages of HCC during tumor progression, and that when the stage increased, there was a lower level of PD-L1 expression. Moreover, HBV infection had no significant influence on PD-L1 or PD-L2 expression in HCC [14]. However, a different study revealed that circulating PD-1/PD-L1 expression was associated with poor prognosis in HBV-related HCC patients following cryoablation [15]. Some preclinical studies in animal models reported that tumor cells in a PD-1 overexpression group grew much slower in a murine hepatocarcinoma model. Moreover, macrophages and cytotoxic T cells were increased in the soluble PD-1-CH50 peptide group because of their ability to inhibit the interaction of PD-1 and PD-L1 [16].
PD-L2 is principally induced through Th-2-associated cytokines. PD-L2 is mainly expressed by antigen-presenting cells, including macrophages, dendritic cells, mast cells, and some B cells, in response to interleukin (IL) 4 and interferon. In contrast, PD-L1 is expressed by a wide variety of immune cells and non-immune cells, as well as most normal tissue cells. The expression of PD-L2 is generally lower than that of PD-L1 [17]. The regulatory pathways of PD-L2 are different from those of PD-L1. The two major pathways that have been reported are the nuclear factor kB pathway and the signal transducer and activator of transcription 6 pathways [18]. Ohaegbulam et al. [4] revealed that PD-L1 and PD-1 binding requires more complex conformational changes than direct binding of PD-L2 to PD-1. Generally, it is known that the binding strength of PD-L2 to PD-1 is three times greater than that of PD-L1. In addition, the simultaneous binding of PD-L1 and L2 to PD-1 has been disproven, implying that the two ligands compete with each other to bind to the receptor [4]. The relationship between PD-L2 and disease prognosis remains controversial. Rozali et al. [17] reported that PD-L2 positive patients had a worse prognosis than negative patients with esophageal carcinoma. However, no correlation with disease free survival was found in many other cancers, including pancreatic, ovarian, and HCC [17]. In our investigation, the overexpression of PD-L2 was found to be correlated with overall survival significantly, but the difference was not statistically significant for DFS. Our results sustained the hypothesis that the PD-L2 in the tumor immune escape differ depending on the status of organ's environments, for example, our cases had very high proportion of HBV and HCV.
Recently, cancer immunotherapies have been highlighted in other malignancies, such as melanoma [8]. Previously, this category was primarily composed of cell-based immunotherapies, such as dendritic, natural killer, and genetically modified T cells, as well as non-cell–based immunotherapy with cytokines, oncolytic viruses, and T-cell checkpoint inhibitors. To date, T-cell checkpoint inhibitors are actively in development for enhancing antitumor immunity [3]. Two papers reporting that the blockade of cytotoxic T lymphocyte antigen-4 (CTLA-4) improved overall survival in metastatic melanoma were recently published [19,20]. In addition, three different checkpoint inhibitors, ipilimumab (anti-CTLA4), pembrolizumab (anti–PD-1), and nivolumab (anti–PD-1), have been approved by the U.S. Food and Drug Administration for melanoma. The drugs have demonstrated great clinical effects on melanoma and non-small cell lung cancer [21]. However, the mechanisms of hepatic carcinogenesis are complex, including genetic, angiogenic, and immunologic factors [3]. Moreover, the liver maintains self-tolerance because it contains specialized cells, such as hepatocytes and dendritic, liver sinusoidal endothelial, Kupffer, hepatic stellate cells, which enhance the secretion of anti-inflammatory cytokines, including IL-10, and transforming growth factor β. These cells induce immunosuppression via the release of such cytokines and by elevating the expression of CTLA-4 and PD-L1 [22]. Although this immunosuppression may contribute to difficulty in targeting HCC, lower toxicity and immunological responses for clinical outcomes have been shown in clinical trials of patients with HCC following treatment with tremelimumab (anti–CTLA-4) [23]. In addition, combination treatments with tumor ablation and nivolumab (anti–PD-1) are ongoing (NCT01658878).
ConclusionIn conclusion, our study demonstrated that the overexpression of PD-Ls in patients with HCC was strongly correlated with overall survival and tumor recurrence. Moreover, PD-Ls are independent prognostic factors for worse overall survival; thus, their overexpression may be a therapeutic target for HCC. However, further multicenter investigations and functional studies are needed to fortify these findings. Accordingly, additional research is warranted to investigate the use PD-Ls as predictive biomarkers for HCC. Moreover, further studies to target PD-1 and PD-Ls in HCC are urgently needed for HCC immunotherapy.
Fig. 1.Immunohistochemical staining of hepatocellular carcinoma tissues using anti–PD-L1 and anti–PD-L2 antibodies. (A-H) Representative staining patterns of hepatocellular carcinoma with negative (A, E), weak intensity (B, F), moderate intensity (C, G), and strong intensity (D, H) staining of PD-L1 (A-D) and PD-L2 (F-H) are shown (×200). PD-L, programmed cell death 1 ligand. 
Fig. 2.Kaplan-Meier survival curves for disease-free survival and overall survival according to PD-L1 (A, B), PD-L2 (C, D), and their combined (E, F) expression status. 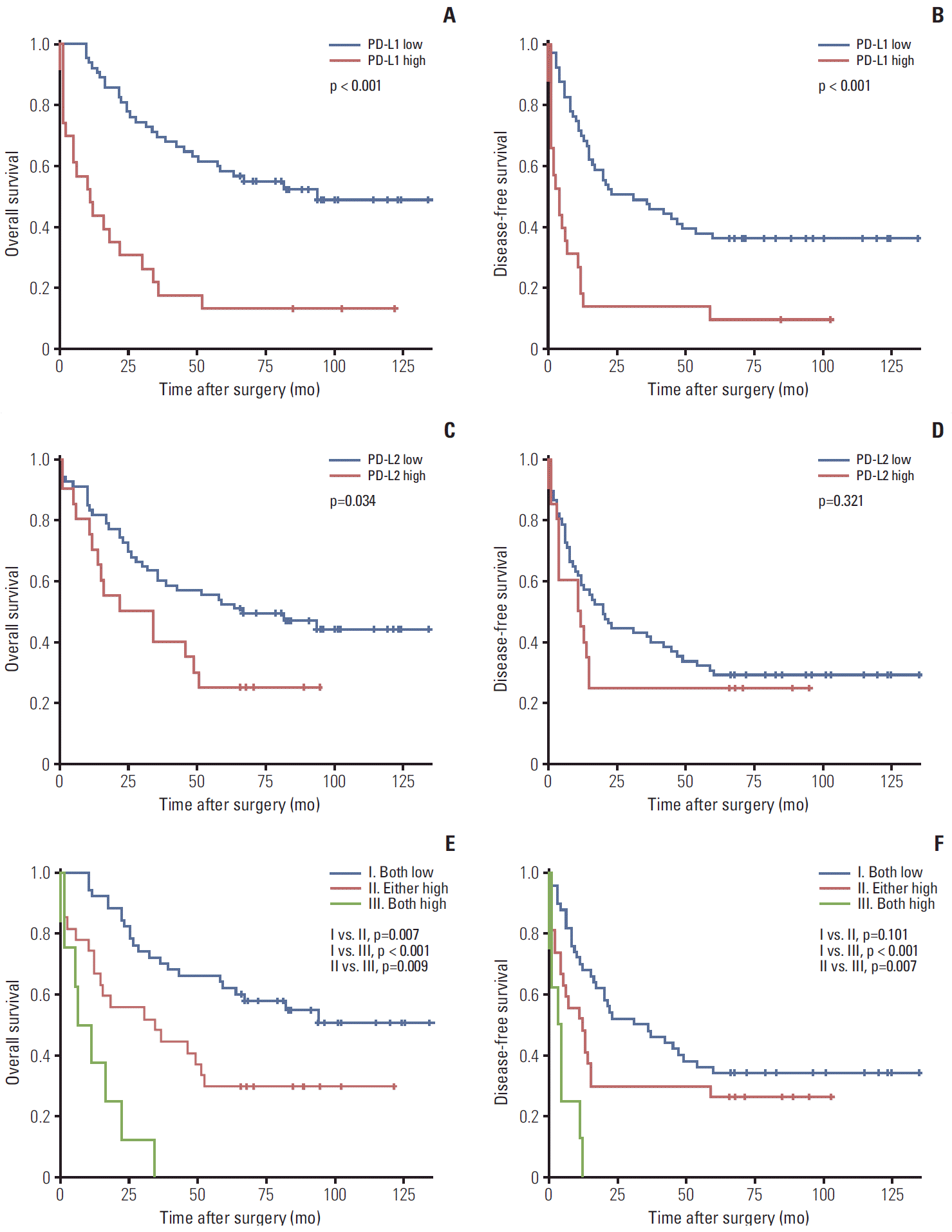
Table 1.Clinicopathologic characteristics and PD-L1 and PD-L2 expression in patients with hepatocellular carcinoma PD-L1, programmed cell death 1 ligand 1; PD-L2, programmed cell death 1 ligand 2; BCLC, Barcelona Clinic Liver Cancer; UICC, the Union Internacional Contra la Cancrum; HBV, hepatitis B virus; HCV, hepatitis C virus; α-FP, α-fetoprotein level; PIVKA-II, protein induced by vitamin K absence or antagonist-II. Table 2.Univariate analysis using the Cox proportional hazard regression model for OS and DFS in patients with hepatocellular carcinoma OS, overall survival; DFS, disease-free survival; HR, hazard ratio; CI, confidence interval; UICC, the Union Internacional Contra la Cancrum; BCLC, Barcelona Clinic Liver Cancer; PD-L1, programmed cell death 1 ligand 1; PD-L2, programmed cell death 1 ligand 2; PD-L, programmed cell death 1 ligand; NA, not acquired. Table 3.Multivariate analysis using the Cox proportional hazard regression model for OS and DFS in patients with hepatocellular carcinoma OS, overall survival; DFS, disease-free survival; HR, hazard ratio; CI, confidence interval; NA, not acquired; UICC, the Union Internacional Contra la Cancrum; BCLC, Barcelona Clinic Liver Cancer; PD-L1, programmed cell death 1 ligand 1; PD-L2, programmed cell death 1 ligand 2; PD-L, programmed cell death 1 ligand. References2. Vilarinho S, Taddei T. Therapeutic strategies for hepatocellular carcinoma: new advances and challenges. Curr Treat Options Gastroenterol. 2015;13:219–34.
3. Sangro B, Palmer D, Melero I. Immunotherapy of hepatocellular carcinoma. Hepat Oncol. 2014;1:433–46.
4. Ohaegbulam KC, Assal A, Lazar-Molnar E, Yao Y, Zang X. Human cancer immunotherapy with antibodies to the PD-1 and PD-L1 pathway. Trends Mol Med. 2015;21:24–33.
5. Ma H, Wey B, Li L. Progress of immunotherapy for hepatocellular carcinoma. Immunogastroenterology. 2013;2:167–72.
6. Qing Y, Li Q, Ren T, Xia W, Peng Y, Liu GL, et al. Upregulation of PD-L1 and APE1 is associated with tumorigenesis and poor prognosis of gastric cancer. Drug Des Devel Ther. 2015;9:901–9.
7. Pan ZK, Ye F, Wu X, An HX, Wu JX. Clinicopathological and prognostic significance of programmed cell death ligand1 (PD-L1) expression in patients with non-small cell lung cancer: a meta-analysis. J Thorac Dis. 2015;7:462–70.
8. Tentori L, Lacal PM, Graziani G. Challenging resistance mechanisms to therapies for metastatic melanoma. Trends Pharmacol Sci. 2013;34:656–66.
9. Thompson RH, Dong H, Lohse CM, Leibovich BC, Blute ML, Cheville JC, et al. PD-1 is expressed by tumor-infiltrating immune cells and is associated with poor outcome for patients with renal cell carcinoma. Clin Cancer Res. 2007;13:1757–61.
10. Nomi T, Sho M, Akahori T, Hamada K, Kubo A, Kanehiro H, et al. Clinical significance and therapeutic potential of the programmed death-1 ligand/programmed death-1 pathway in human pancreatic cancer. Clin Cancer Res. 2007;13:2151–7.
11. Hamanishi J, Mandai M, Iwasaki M, Okazaki T, Tanaka Y, Yamaguchi K, et al. Programmed cell death 1 ligand 1 and tumor-infiltrating CD8+ T lymphocytes are prognostic factors of human ovarian cancer. Proc Natl Acad Sci U S A. 2007;104:3360–5.
12. McDermott DF, Atkins MB. PD-1 as a potential target in cancer therapy. Cancer Med. 2013;2:662–73.
13. Gao Q, Wang XY, Qiu SJ, Yamato I, Sho M, Nakajima Y, et al. Overexpression of PD-L1 significantly associates with tumor aggressiveness and postoperative recurrence in human hepatocellular carcinoma. Clin Cancer Res. 2009;15:971–9.
14. Wang BJ, Bao JJ, Wang JZ, Wang Y, Jiang M, Xing MY, et al. Immunostaining of PD-1/PD-Ls in liver tissues of patients with hepatitis and hepatocellular carcinoma. World J Gastroenterol. 2011;17:3322–9.
15. Zeng Z, Shi F, Zhou L, Zhang MN, Chen Y, Chang XJ, et al. Upregulation of circulating PD-L1/PD-1 is associated with poor post-cryoablation prognosis in patients with HBV-related hepatocellular carcinoma. PLoS One. 2011;6:e23621
16. He L, Zhang G, He Y, Zhu H, Zhang H, Feng Z. Blockade of B7-H1 with sPD-1 improves immunity against murine hepatocarcinoma. Anticancer Res. 2005;25:3309–13.
17. Rozali EN, Hato SV, Robinson BW, Lake RA, Lesterhuis WJ. Programmed death ligand 2 in cancer-induced immune suppression. Clin Dev Immunol. 2012;2012:656340.
18. Huber S, Hoffmann R, Muskens F, Voehringer D. Alternatively activated macrophages inhibit T-cell proliferation by Stat6-dependent expression of PD-L2. Blood. 2010;116:3311–20.
19. Hamid O, Robert C, Daud A, Hodi FS, Hwu WJ, Kefford R, et al. Safety and tumor responses with lambrolizumab (anti-PD-1) in melanoma. N Engl J Med. 2013;369:134–44.
20. Topalian SL, Hodi FS, Brahmer JR, Gettinger SN, Smith DC, McDermott DF, et al. Safety, activity, and immune correlates of anti-PD-1 antibody in cancer. N Engl J Med. 2012;366:2443–54.
|
|
|||||||||||||||||||||||||||||||||||||||||