AbstractPurposeConcurrent chemoradiation (CRT) with 3-weekly doses of cisplatin is a standard treatment for loco-regionally advanced head and neck squamous cell carcinoma (HNSCC). However, treatment with 3-weekly doses of cisplatin is often associated with several adverse events. Therefore, we conducted this retrospective analysis to determine the efficacy and tolerance of CRT with a low weekly dose of cisplatin in stage IV HNSCC patients.
Materials and MethodsMedical records of patients who were diagnosed with stage IV HNSCC and received concurrent CRT were analyzed. All patients were treated weekly with cisplatin at 20-30 mg/m2 until radiotherapy was completed.
ResultsA total of 35 patients were reviewed. Median follow up was 10.7 months (range, 1.7 to 90.5 months), the median radiation dose was 7,040 cGy, and the median dose of cisplatin received was 157 mg/m2. Eleven patients received docetaxel combination chemotherapy. Overall, 25 patients (71.4%) achieved complete response (CR), eight (22.9%) showed partial response. The median overall survival was 42.7 months, the 3-year survival rate was 51.2% and the 3 year disease-free survival rate was 72.8%. Overall survival was improved in patients who achieved CR relative to others (59.7 months vs. 13.4 months; p=0.008). There were significant differences in survival between patients who received docetaxel combination and cisplatin alone (51.8 months vs. 7.9 months; p=0.009). Grade 3-4 adverse events included stomatitis (82.9%), dermatitis (22.9%), infection (11.4%), dysphagia (8.6%), and neutropenia (5.7%).
IntroductionLocally advanced head and neck squamous cell carcinoma (HNSCC) is currently treated with concurrent chemoradiation (CRT) or surgery followed by postoperative radiotherapy [1,2]. Compared with surgery, concurrent CRT can preserve the function of the vocal cord and maintain the structure of the neck. Accordingly, CRT has become a standard modality for this disease [3,4].
Cisplatin is one of the most commonly used and best-studied drugs for CRT. Treatment with a single-agent bolus of cisplatin every 3 weeks at a dose of 100 mg/m2 is accepted as the standard regimen [2,5]. However, this regimen is associated with significant acute and late adverse events such as mucositis, hematological complications, and renal complications [5-7]. Additionally, the completion rate for this regimen is relatively poor [2,5]. Therefore, splitting the 3-weekly cisplatin into a weekly cisplatin schedule might decrease toxicities and increase compliance. Several studies have suggested CRT with a weekly cisplatin regimen would be successful for treatment of locally advanced HNSCC [8-11].
Locally advanced stage IV HNSCC has an especially poor prognosis with a high local or systemic recurrence rate [12]. The complete response rate of stage IV HNSCC is expected to be lower than that of stage II or III of the same disease.
In this study, we retrospectively analyzed stage IV HNSCC patients who were treated with concurrent CRT with low-dose weekly cisplatin. The goal of this study was to evaluate the efficacy, feasibility, and toxicity profile of the low-dose weekly cisplatin regimen.
Materials and Methods1. Data collectionWe retrospectively reviewed data describing patients with histologically confirmed HNSCC who were treated at Gyeongsang National University Hospital between 2005 and 2012. All patients were staged according to the 2002 American Joint Committee on Cancer staging system and were diagnosed with stage IV disease. The staging techniques used were as follows: contrast-enhanced computed tomography (CT) of the neck, chest, and abdomen; positron emission tomography (PET)-CT; and pan-endoscopy. Electronic medical records were reviewed for demographic and clinical characteristics, including age, gender, Eastern Cooperative Oncology Group (ECOG) performance score, stage of disease, and tumor location. Treatment, follow-up, and death records were identified using the hospital-based electronic medical record system.
2. Chemoradiation protocolIntravenous cisplatin was administered at days 1, 8, and 15 every 4 weeks during radiotherapy (weeks 1, 2, 3, 5, 6, and 7). A single cisplatin dose was 30 mg/m2, and the designated full-intended dose of cisplatin was 180 mg/m2. Eleven patients were administered combined chemotherapy with docetaxel and cisplatin at a dose of 20 mg/m2. Prehydration and posthydration with normal saline were administered using a standard oncology protocol. Anti-emetic prophylaxis with 5HT3-antagonists and dexamethasone was administered using a standard oncology protocol. All patients received 70-72 Gy in 30-35 fractions over 7 weeks. The treatment was planned using a CT simulator and a 3-dimensional dose-calculation computer.
3. Response and toxicity assessmentFor measurable lesions, the response to therapy was assessed by clinical examination and CT and/or PET-CT imaging 6-8 weeks after the completion of chemoradiation using the Response Evaluation Criteria in Solid Tumors (RECIST). Regular imaging (CT or magnetic resonance imaging) follow-up was performed for response evaluation, then every 3 months during the first 2 years and every 6 months thereafter. PET-CT was performed after 2 months of treatment, then annually. If a lesion could not be clearly distinguished as a residual tumor or treatment-related scar change and remained stable over time with no signs or symptoms of disease it was considered to be ‘progression free.’
Treatment-related toxicities were graded using the Common Terminology Criteria for Adverse Events (NCICTCAE) ver. 3.0. Hematologic and non-hematologic adverse events were evaluated during treatment. At the end of treatment, long-term adverse events such as xeroderma, dysphagia, and neck fibrosis were evaluated.
4. Statistical analysisStatistical analysis was performed using PASW ver. 18 (SPSS Inc., Chicago, IL, USA). Survival analysis was carried out using the Kaplan-Meier method. Overall survival (OS) was defined as the time from the date of diagnosis of the cancer to the date of death from any cause. Cases of persistent or recurrent primary disease after the completion of CRT were considered to be local failures. Disease-free survival (DFS) was defined as the time from the date of a confirmed complete response to the date of recurrence. Progression-free survival (PFS) was defined as the time from diagnosis until tumor relapse or progression or death from any cause.
ResultsBetween 2005 and 2012, 46 patients with histologically confirmed HNSCC were treated with CRT. Of these, 35 were locally advanced stage IV patients who were eligible for analysis. The patients’ characteristics are shown in Table 1. There were no females (males, 35 patients; 100%), and the median age of patients was 65 years (range, 34 to 82 years). The performance status of patients was relatively good, and all had a status of 0 or 1 (25.7% and 74.3%, respectively). The oropharynx and hypopharynx were the most common sites (42.9% and 40.0%, respectively). Regarding those patients diagnosed before January 2012, only 10 had undergone DNA testing for human papillomavirus (HPV) because the HPV examination was not available at our hospital.
1. Treatment outcomesThe median follow-up duration was 10.7 months (range, 1.7 to 90.5 months). Twenty-four patients received cisplatin alone, while 11 received the combined regimen with docetaxel. The median total dose of actually received cisplatin was 157 mg/m2, and 16 patients received a modified dose and schedule. Nineteen patients completed the initially planned chemotherapy dose and schedule. The causes of modification were poor performance (n=8, 22.9%), and cytopenia, infection, and renal dysfunction (n=3, 8.6%, each). The median dose of radiation was 7,040 cGy (range, 3,200 to 7,200 cGy).
The chemoradiation results are described in Table 2. A complete response (CR) was achieved in 25 patients with a CR rate of 71.4%. The disease control rate (including complete, partial responses, and stable disease) was 97.1%, and 34 of 35 patients achieved at least stable disease (SD). Of patients who initially achieved CR, six were confirmed to have disease recurrence with a recurrence rate of 24% (6/25). Two of eight patients who achieved partial response (PR) received salvage surgery, one achieved remission with no evidence of disease and another recurred and expired because of disease progression.
The median OS was 42.7 months, and the 3-year survival rate was 51.2% (Fig. 1). The DFS did not reach the median value, and the 3-year DFS rate was 72.8% (Fig. 2). OS was improved in patients who achieved CR relative to others (59.7 months vs. 13.4 months, respectively; p=0.008) (Fig. 3). There were significant differences in survival between docetaxel combination and cisplatin alone (51.8 months vs. 7.9 months; p=0.009). The initial response was also important to overall survival. Patients who achieved at least PR showed better prognosis (CR or PR vs. SD or progressive disease, 31.5 months vs. 3.5 months; p<0.001). Multivariate analyses were not conducted because the number of patients was too small to achieve statistical significance.
2. Toxicity profilesTreatment-related adverse events are shown in Table 3. Only one patient expired during chemoradiation due to severe pneumonia. Stomatitis and skin dermatitis were the most common grade III adverse events (n=29 [82.9%] and n=8 [22.9%], respectively). Patients who experienced severe stomatitis were managed with oral gargle and analgesics. In this retrospective study, most grade III stomatitis patients continued to radiation, but with a modified dose and schedule of cisplatin. Few patients experienced infection and dysphagia. However, one patient experienced grade III renal dysfunction and another grade IV emesis. Hematologic adverse events were generally tolerable and manageable.
If adverse events persisted for more than 6 months after the completion of chemoradiation, they were considered to be persistent adverse events. Grade III persistent adverse events comprised only two cases of xerostomia.
DiscussionIn locally advanced HNSCC, 3-weekly cisplatin treatments at a dose of 100 mg/m2 concurrent with radiotherapy is considered to be the standard treatment based on several phase III trials [2,5]. However, the reported rate of high-grade adverse events ranged from 77% to 85% for high-dose cisplatin [5,13]. Mucositis, dysphagia, and emesis are common adverse events of chemoradiotherapy of HNSCC. Additionally, renal toxicity of high-dose cisplatin is a not uncommon, but critical event, that occurred with an incidence of 5%-8% in previous trials [2,5,6]. The completion rate of this high-dose cisplatin regimen has been reported to be relatively low, with 63%-85% of patients in the CRT arm completing the planned cycles of CRT in several clinical trials [5,6].
Modification of schedules and reduction of the dose of cisplatin have been investigated for their potential to decrease toxicity, but no randomized trials have evaluated 100 mg/m2 cisplatin. Chan et al. [14] reported that CRT using weekly cisplatin at a dose of 40 mg/m2was well tolerated in patients with advanced nasopharyngeal carcinoma. A Japanese study reported a retrospective analysis at a dose of 40 mg/m2 on weeks 1, 2, 3, 5, 6, and 7 of the radiotherapy schedule in stage II-IV HNSCC [15]. The CR rate was 98.1%, and the 2-year OS and local PFS rates were 93.7% and 88.0%, respectively. Espeli et al. [16] and Otty et al. [17] also conducted single center retrospective studies of CRT with weekly cisplatin in stage II-IV HNSCC. According to these studies, CRT with weekly cisplatin in stage II-IV HNSCC showed less toxicity and acceptable efficacy. Table 4 shows a comparison of single center retrospective analyses. Survival rates were similar in our study, which included only stage IV disease, to others that included patients with stages II-IV [15,17,18].
Several studies have established that weekly cisplatin is effective and less toxic. However, the present study is the first report of HNSCC patients in a far-advanced stage (IVa and IVb). Considering that the patients in our study all had stage IV disease, the response rate and OS did not seem to be inferior to other trials. In addition, our study is the first report in South Korea.
Mucositis was the most common severe adverse event in the present study. The incidences of grade III mucositis and dermatitis were higher than in other similar trials. This may be related to the greater tumor volume in our study population. However, the incidences of emesis and renal toxicity were lower, and there were manageable hematological adverse events. Particularly, fewer persistent adverse events were reported in our study, and only two cases of xerostomia were reported. The lower total cumulative dose of cisplatin used may be related to the mild long-term toxicities.
It should be noted that this study had several limitations. First, it was a single-center, retrospective analysis of a small number of patients. In addition, not all patients were treated with the same dose and chemotherapeutic agent, some received a reduced dose of cisplatin and combined treatment with another agent (docetaxel). Therefore, the chemotherapeutic protocol was not homogeneous. Treatment outcomes showed significant differences in overall survival between chemotherapeutic agents. However, the number of patients who received docetaxel was too small to assess survival; therefore, multivariate analysis was not available in our study. Furthermore, some bias might have existed due to the inclusion of patients with relatively good performance status.
Owing to the small number of patients, it is difficult to place great significance on the results of the multivariate analysis. However, the standard protocol produced the expected toxicity, and low-dose weekly cisplatin protocol showed acceptable efficacy and toxicity in far-advanced-stage HNSCC patients.
ConclusionIn conclusion, the present study showed that chemoradiotherapy with low-dose weekly cisplatin had an acceptable response relative to the previous standard protocol of 3-weekly treatments with cisplatin, and appeared to reduce the incidence of severe adverse events, particularly long-term toxicities such as xerostomia. CRT with low-dose weekly cisplatin is thus likely effective and tolerable, even in patients with locally advanced-stage IV HNSCC. Further, well-designed trials in comparison with the standard 3-weekly cisplatin regimen are warranted.
Fig. 2.Disease-free survival. Disease-free survival does not reach median; 3-year disease-free survival is 72.8%. 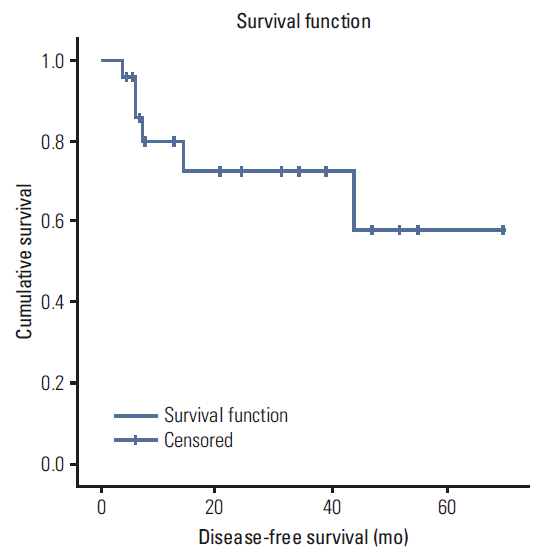
Table 1.Baseline patient and tumor characteristics Table 2.Response according to staging and recurrent cases in CR cases
Table 3.Adverse events
Table 4.Comparisons of previous studies
References1. Pignon JP, Bourhis J, Domenge C, Designe L. Chemotherapy added to locoregional treatment for head and neck squamouscell carcinoma: three meta-analyses of updated individual data. MACH-NC Collaborative Group. Meta-analysis of chemotherapy on head and neck cancer. Lancet. 2000;355:949–55.
2. Forastiere AA, Goepfert H, Maor M, Pajak TF, Weber R, Morrison W, et al. Concurrent chemotherapy and radiotherapy for organ preservation in advanced laryngeal cancer. N Engl J Med. 2003;349:2091–8.
3. Budach W, Hehr T, Budach V, Belka C, Dietz K. A meta-analysis of hyperfractionated and accelerated radiotherapy and combined chemotherapy and radiotherapy regimens in unresected locally advanced squamous cell carcinoma of the head and neck. BMC Cancer. 2006;6:28.
4. Traynor AM, Richards GM, Hartig GK, Khuntia D, Cleary JF, Wiederholt PA, et al. Comprehensive IMRT plus weekly cisplatin for advanced head and neck cancer: the University of Wisconsin experience. Head Neck. 2010;32:599–606.
5. Adelstein DJ, Li Y, Adams GL, Wagner H Jr, Kish JA, Ensley JF, et al. An intergroup phase III comparison of standard radiation therapy and two schedules of concurrent chemoradiotherapy in patients with unresectable squamous cell head and neck cancer. J Clin Oncol. 2003;21:92–8.
6. Al-Sarraf M, Pajak TF, Marcial VA, Mowry P, Cooper JS, Stetz J, et al. Concurrent radiotherapy and chemotherapy with cisplatin in inoperable squamous cell carcinoma of the head and neck: an RTOG Study. Cancer. 1987;59:259–65.
7. Machtay M, Moughan J, Trotti A, Garden AS, Weber RS, Cooper JS, et al. Factors associated with severe late toxicity after concurrent chemoradiation for locally advanced head and neck cancer: an RTOG analysis. J Clin Oncol. 2008;26:3582–9.
8. Ho KF, Swindell R, Brammer CV. Dose intensity comparison between weekly and 3-weekly cisplatin delivered concurrently with radical radiotherapy for head and neck cancer: a retrospective comparison from New Cross Hospital, Wolverhampton, UK. Acta Oncol. 2008;47:1513–8.
9. Steinmann D, Cerny B, Karstens JH, Bremer M. Chemoradiotherapy with weekly cisplatin 40 mg/m(2) in 103 head-and-neck cancer patients: a cumulative dose-effect analysis. Strahlenther Onkol. 2009;185:682–8.
10. Jeremic B, Shibamoto Y, Stanisavljevic B, Milojevic L, Milicic B, Nikolic N. Radiation therapy alone or with concurrent low-dose daily either cisplatin or carboplatin in locally advanced unresectable squamous cell carcinoma of the head and neck: a prospective randomized trial. Radiother Oncol. 1997;43:29–37.
11. Huguenin P, Beer KT, Allal A, Rufibach K, Friedli C, Davis JB, et al. Concomitant cisplatin significantly improves locoregional control in advanced head and neck cancers treated with hyperfractionated radiotherapy. J Clin Oncol. 2004;22:4665–73.
12. Parkin DM, Bray F, Ferlay J, Pisani P. Global cancer statistics, 2002. CA Cancer J Clin. 2005;55:74–108.
13. Cooper JS, Pajak TF, Forastiere AA, Jacobs J, Campbell BH, Saxman SB, et al. Postoperative concurrent radiotherapy and chemotherapy for high-risk squamous-cell carcinoma of the head and neck. N Engl J Med. 2004;350:1937–44.
14. Chan AT, Leung SF, Ngan RK, Teo PM, Lau WH, Kwan WH, et al. Overall survival after concurrent cisplatin-radiotherapy compared with radiotherapy alone in locoregionally advanced nasopharyngeal carcinoma. J Natl Cancer Inst. 2005;97:536–9.
15. Homma A, Inamura N, Oridate N, Suzuki S, Hatakeyama H, Mizumachi T, et al. Concomitant weekly cisplatin and radiotherapy for head and neck cancer. Jpn J Clin Oncol. 2011;41:980–6.
16. Espeli V, Zucca E, Ghielmini M, Giannini O, Salatino A, Martucci F, et al. Weekly and 3-weekly cisplatin concurrent with intensity-modulated radiotherapy in locally advanced head and neck squamous cell cancer. Oral Oncol. 2012;48:266–71.
|
|
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||