A Retrospective Study of First-Line Combination Chemotherapy in Advanced Colorectal Cancer: A Korean Single-Center Experience
Article information
Abstract
Purpose
Fluoropyrimidine-based combination chemotherapy, in combination with either oxaliplatin or irinotecan, has demonstrated efficacy and tolerability in treatment of advanced colorectal cancer (ACC).
Materials and Methods
Between January 2006 and December 2007, a total of 478 ACC patients were treated with combination chemotherapy in first-line settings. Combination therapies included: 5-fluorouracil, folinic acid plus oxaliplatin (FOLFOX, n=172), 5-fluorouracil, folinic acid plus irinotecan (FOLFIRI, n=95), capecitabine plus oxaliplatin (XELOX, n=155), and capecitabine plus irinotecan (XELIRI, n=56). FOLFOX and FOLFIRI were repeated every 2 weeks, whereas XELOX and XELIRI were repeated every 3 weeks until occurrence of disease progression or unacceptable toxicity, or until a patient chose to discontinue treatment.
Results
The median age was 58 years (range, 19 to 84 years) and the median chemotherapy durations for FOLFOX, FOLFIRI, XELOX, and XELIRI were 4.9, 4.5, 5.7, and 5.4 months, respectively. Combination chemotherapy regimens were generally well tolerated. The estimated median progression-free-survival (PFS) for all patients was 6.8 months (95% confidence interval, 6.3 to 7.3 months). No statistically significant difference in PFS was found among regimens used as first-line chemotherapy. Sixty percent (n=290) of patients received second or further lines of therapy after failure.
Conclusion
Fluoropyrimidine-based combination chemotherapy regimens appear to be equally active and tolerable as first-line therapy for ACC.
Introduction
Colorectal adenocarcinoma is the fourth most frequently diagnosed malignancy in Korea, accounting for 12% of newly diagnosed cancer cases. According to the Ministry of Health and Welfare, the incidence of colorectal cancer has increased in both males and females during the past 2 decades [1]. Although surgery is potentially curative, approximately one third of all newly diagnosed patients present with inoperable metastatic disease. Palliative chemotherapy is more effective than the best supportive care for improving overall survival (OS) as well as quality of life in advanced colorectal cancer [2]. While significant advances have been made in recent years, cure is rarely possible in advanced colorectal cancer (ACC), making further improvements in therapy imperative. For more than three decades, the treatment options for ACC have been almost exclusively based on 5-fluorouracil (5-FU) and folinic acid (FA) [3]. Until the early 1990s, 5-FU, often modulated by FA, was the single effective chemotherapy available, but only led to meaningful responses in a small minority of treated patients. The recent integration of oxaliplatin and irinotecan for the management of ACC patients has extended median OS in a meaningful way. Both drugs have been shown to have synergistic effects with 5-FU and FA in colorectal cancer cell lines [4,5]. Since irinotecan and oxaliplatin have been used for ACC treatment, the efficacy of palliative chemotherapy for ACC has considerably improved.
First-line treatment with irinotecan and either bolus or infusional 5-FU/FA, namely irinotecan/bolus fluorouracil/LV or 5-fluorouracil, folinic acid plus irinotecan (FOLFIRI), significantly improved outcomes as compared with 5-FU/FA [6,7]. Similarly, a combination of oxaliplatin and infusional 5-FU/FA, known as 5-fluorouracil, folinic acid plus oxaliplatin (FOLFOX), significantly increased the response rate and the time to progression compared with 5-FU/FA [8]. These results established 5-FU-based chemotherapy, in combination with either irinotecan or oxaliplatin, as standard first-line chemotherapy regimens for patients with ACC.
Capecitabine is an oral fluoropyrimidine designed to mimic a continuous infusion of 5-FU. Capecitabine is considered to be as effective and more tolerable than 5-FU [9]. Furthermore, capecitabine has been shown to exhibit antitumor activity against ACC both as a single agent [10,11] and in combination with oxaliplatin [12-14], as well as with irinotecan [15]. In Korea, capecitabine was approved in January 2006 as a partner with oxaliplatin or irinotecan for the treatment of ACC.
A decision regarding chemotherapy regimens for an individual patient can be a common clinical situation. Factors considered include the extent of disease, potential toxicities, especially for those with impaired oral intake or with decreased performance status, activity of chemotherapy, and the patient preference. The present evaluation was done to plan and develop optimal treatment for Korean patients. We therefore decided to evaluate various combination chemotherapy regimens as first-line chemotherapy for ACC.
Materials and Methods
This report describes a single-center, retrospective study. Between January 2006 and December 2007, a total of 537 ACC patients were treated with first-line chemotherapy for advanced disease at Samsung Medical Center (Seoul, Korea). Fifty-nine patients were excluded because they were treated with single-agent chemotherapy. The criteria for case inclusion were as follows; 1) histologically confirmed diagnosis of adenocarcinoma arising from colon or rectum, 2) no prior chemotherapy or radiotherapy except for adjuvant use, 3) advanced (metastatic and/or recurrent) disease, 4) availability of clinical data at the beginning of therapy and follow-up. We attempted to exclude patients who were enrolled in clinical trials to ensure the choice of chemotherapy regimen was solely at the discretion of the treating physician. We collected follow-up patient data from the Samsung Medical Center cancer registry. All the data were prospectively recorded and only the survival data was updated at the time of analysis. Written informed consent was given by all patients prior to receiving chemotherapy, according to institutional guidelines. Approval of the study was obtained from the Institutional Review Board.
The patients were required to have a life expectancy of 12 weeks of more; age of at least 18 years or older; Eastern Cooperative Oncology Group (ECOG) performance status of 2 or lower; adequate hematologic (neutrophil count>1,500/mm3 and platelet count>100,000/mm3), hepatic (serum total bilirubin level<1.5 mg/dL and aspartate aminotransferase/alanine aminotransferase<3×upper limit normal) and renal (serum creatinine level<1.5 mg/dL) functions. Our department guidelines define combination chemotherapy regimens as follows: In FOLFOX or FOLFIRI, FA is given at the dose of 200 mg/m2 followed by bolus 5-FU 400 mg/m2 on day 1, and a 46-hour continuous infusion of 5-FU 2,400 mg/m2 on days 1 and 2. Oxaliplatin 85 mg/m2 or irinotecan 180 mg/m2 was administered on day 1 as a 2-hour infusion, concurrent with FA. In capecitabine plus oxaliplatin (XELOX) and capecitabine plus irinotecan (XELIRI), oxaliplatin 130 mg/m2 or irinotecan 240 mg/m2 was given on day 1 in combination with oral capecitabine 1,000 mg/m2 twice daily on days 1 to 14. FOLFOX and FOLFIRI were repeated every 2 weeks, whereas XELOX and XELIRI were repeated every 3 weeks until disease progression or unacceptable toxicity occurred, or until a patient chose to discontinue treatment. The dosages for subsequent cycles were adjusted according to the toxic effects that developed during the preceding cycle. All patients received a standard supportive regimen consisting of hydration and antiemetics. The prophylactic use of hematopoietic growth factors was not allowed during treatment, except for patients with febrile neutropenia or grade 4 myelosuppression at the treating physician's discretion. After this combination chemotherapy had failed, second-line chemotherapy was recommended to all the patients if their performance status was preserved. According to department policies, all tumor measurements were assessed every 2 or 3 cycles of chemotherapy by using an abdominopelvic computed tomography (CT) scan and other tests that were initially used to stage the tumor. Tumor response and progression were evaluated according to the Response Evaluation Criteria for Solid Tumors (RECIST) [16]. Toxicity grading was based on the National Cancer Institute Common Toxicity Criteria (ver. 3).
The primary endpoint of this retrospective study was progression-free survival (PFS). OS, response rate and tolerability were secondary endpoints. The starting point of PFS was the first day of chemotherapy. The date of disease progression or death from causes other than ACC was used in calculating PFS. PFS and OS were estimated according to the Kaplan-Meier method and the statistical significance of differences in survival curves between groups was tested with a log-rank test. Multivariate models were used for exploratory purposes to examine the impact of each regimen on the outcomes of chemotherapy. Covariates included were age (below vs.≥median), gender, previous adjuvant therapy, an ECOG performance status (0-1 vs.≥2), number of involved sites (1 vs.≥2), metastases (liver, peritoneum, and lung), baseline chemistry profiles (serum albumin, alkaline phosphatase, and bilirubin), combination with bevacizumab, and chemotherapy regimens. Laboratory parameters were initially recorded as continuous variables and later dichotomized according to the median value of each variable (below vs.≥median). All p-values were two-sided, with p<0.05 indicating statistical significance.
Results
Between January 2006 and December 2007, a total of 478 ACC patients were treated with combination chemotherapy in a first-line setting: FOLFOX (n=172), FOLFIRI (n=95), XELOX (n=155), and XELIRI (n=56). In 29 patients, chemotherapy involved bevacizumab. Baseline characteristics were balanced between patients treated with each regimen (Table 1). The median age was 58 years with a range of 19-84 years. Sixty percent of patients were male, and 33 patients (7%) had an ECOG performance status of 2 or more. More than half of the patients (n=263) had received surgery for curative intent, and 206 patients received adjuvant chemotherapy or chemoradiotherapy. Approximately one-third of the patients had two or more metastatic disease sites, mostly involving liver and abdominal lymph nodes. We noted that more FOLFIRI or XELIRI patients had received adjuvant therapy involving oxaliplatin than FOLFOX or XELOX patients. After first-line failure, second-line chemotherapy was administered for more than half of the patients (n=290). Median follow-up duration was 40.6 months (95% confidence interval [CI], 39.3 to 41.8 months). At the time of data collection, 449 (89%) patients had progressed and 190 (40%) were known to have died.
Median chemotherapy durations for FOLFOX, FOLFIRI, XELOX, and XELIRI were 4.9, 4.5, 5.7 and 5.4 months, respectively. We found no statistically significant difference among chemotherapy durations for these regimens (log-rank p=0.19). The most common reason for discontinuation of treatment was disease progression. In 172 patients receiving FOLFOX, two-thirds of patients discontinued therapy due to disease progression (n=118), physician's recommendation or patient withdrawal (n=33), or toxicity (n=21). FOLFIRI patients discontinued therapy due to progression (n=60), physician's recommendation or patient withdrawal (n=13), toxicity (n=20), or unknown causes (n=2). Similarly, disease progression was the most common cause of therapy discontinuation in 101 XELOX patients and 34 XELIRI patients.
Overall, all of the combination chemotherapy regimens were generally well tolerated. We found no relevant difference in the occurrence of overall grade 3 or 4 toxicities among regimens (Table 2). In brief, the main difference in grade 3 or 4 toxicities with FOLFIRI or XELIRI was diarrhea (21% for FOLFIRI and 27% for XELIRI vs. 11% for FOLFOX and 9% for XELOX; p=0.02), and with FOLFOX or XELOX the difference involved peripheral neuropathy (9% for FOLFOX and 7% for XELOX vs. 2% for FOLFIRI and XELIRI; p<0.01). Although patients who were treated with irinotecan-containing chemotherapy more frequently experienced grade 3 or 4 leukopenia (13% vs. 10%; p=0.09) than those treated with oxaliplatin-containing regimens, we found no significant difference in the incidence of febrile neutropenia (5% in each arm). In addition, grade 2 or more hand-foot syndrome was more frequently observed in XELOX and XELIRI (14% and 12%, respectively) than in FOLFOX and FOLFIRI (6% and 8%, respectively). In the current retrospective analysis, seven possible treatment-related deaths were identified. One death occurred in the midst of treatment with FOLFOX, with no clinical evidence of progression having been demonstrated. Another patient died of respiratory failure shortly after completion of the second FOLFOX cycle, in which the possibility of disease progression could not be completely excluded. The patient, initially presenting with multiple pulmonary nodules and bilateral pleural effusion, complained about increasing dyspnea and suffered a sudden respiratory arrest. Five other deaths occurred in patients while receiving FOLFIRI or XELOX, and were attributed to neutropenic sepsis.
Of a total of 478 patients, 61 could not be evaluated for responses because of the absence of any measurable lesions or early discontinuation of therapy. Objective responses to chemotherapy were noted in 200 patients (response rate, 48%; 95% CI, 43 to 53%); 42% for FOLFOX, 49% for FOLFIRI, 55% for XELOX, and 51% for XELIRI. The difference in the response rates for each regimen was not statistically significant (p=0.09). Patients who had a poor performance status (≥2 in ECOG scale) were significantly less likely to respond to first-line chemotherapy (24% vs. 50%; p<0.01) compared to those with an ECOG performance status of 0 or 1. Response rate was not significantly influenced by age, gender, prior treatments, baseline laboratory parameters, metastatic sites, or chemotherapy regimen. Also, combination of bevacizumab did not affect response rate.
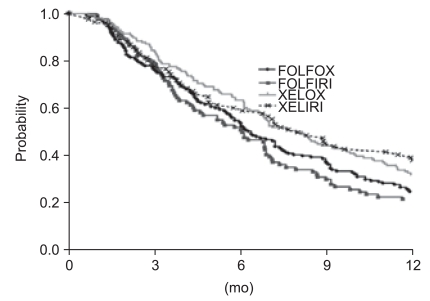
The estimated median PFS for all patients was 6.8 months (95% CI, 6.3 to 7.3 months), and the median OS was not yet reached. PFS was shorter, although statistically insignificant (p=0.12), in patients receiving FOLFOX or FOLFIRI (6.2 months and 6.0 months, respectively) than those receiving XELOX (7.9 months) or XELIRI (7.1 months). Chemotherapy outcomes are summarized in Table 3. One-year PFS rates for FOLFOX, FOLFIRI, XELOX, and XELIRI were 24%, 21%, 32%, and 32%, respectively (Fig. 1). A multivariate regression model revealed that PFS was significantly affected by performance status (hazard ratio, 0.39; 95% CI, 0.28 to 0.57; p<0.01). We also tested whether the PFS was modified by interaction between the effect of baseline clinical parameters and the chemotherapy regimens; the first-level interaction term between these variables was entered into a separate multivariate model. However, we found no interaction between any first-line chemotherapy regimens for each clinical parameter.
Discussion
Despite recent advances in the treatment of ACC [17], patients treated with first-line chemotherapy have a median OS rarely exceeding 24 months. In the current analysis, outcomes for ACC are comparable to those in the published trials of combination chemotherapy. There appears to be no advantage of one combination regimen over the others. Our observation that PFS was slightly shorter with FOLFOX or FOLFIRI than with XELOX or XELIRI is possibly related to negative prognostic factors influencing the choice of intravenous chemotherapeutic agents instead of oral agents. ACC patients who already had peritoneal dissemination seldom could tolerate oral agents. Similarly, the choice of a chemotherapeutic agent depends on the ones previously used in the adjuvant setting. Although this study is retrospective in nature, the results provide a piece of evidence that patients with ACC may derive an indisputable benefit from fluoropyrimidine-based combination chemotherapy. The decision to use specific chemotherapeutic agent(s) in patients with ACC should be determined by their relative merits on a case-by-case basis.
The evolution of treatment using irinotecan and oxaliplatin in combination with 5-FU regimens has resulted in a significant prolongation of life in patients with ACC. Since both drugs have demonstrated similar activity in first- and second-line settings, the optimal chemotherapy regimen and dosing schedule in patients with ACC remains undecided [18]. Randomized trials comparing first-line FOLFOX with FOLFIRI indicated equivalent activity and moderate toxicity differences between these two regimens [19], suggesting that use of either oxaliplatin or irinotecan is reasonable. In another phase III study in which patients crossed over to the alternative regimen upon progression while on their first-line regimen, the overall PFS on first-line therapy was 8.1 months for FOLFOX and 8.5 months for FOLFIRI [20]. In a combined analysis of seven phase III trials in ACC, Grothey et al. [21] reported that the strategy of making these three active drugs (fluoropyrimidine, oxaliplatin, and irinotecan) available to patients with ACC could maximize OS.
In addition to efficacy data, patient convenience and satisfaction are assuming increased importance in cancer management. Oral administration has the advantage of permitting convenient, patient-orientated therapy, providing the patient with a degree of independence and improved quality of life, while avoiding complications associated with intravenous drug administration. Furthermore, most patients prefer orally administered therapy to intravenous treatment [22]. Chemotherapy regimens involving oral capecitabine showed similar safety and efficacy profiles compared with 5-FU-based regimens [23]. Oral capecitabine was proved to have a similar quality of life profile to that of 5-FU [24], but seemed to be more convenient in terms of administration.
In Korea, a capecitabine-containing regimen was approved in January 2006 as the first-line treatment of ACC. Data from the current retrospective study suggest that patients are highly compliant with capecitabine, when given in combination with either oxaliplatin or irinotecan. Response rates and PFS were similar between FOLFOX/FOLFIRI and XELOX/XELIRI. Patients treated with capecitabine experienced a higher incidence of clinically relevant hand-foot syndrome, but this toxic effect was predictable and manageable.
An improved understanding of the molecular pathogenesis of cancer has lead to the development of novel agents designed to target critical cellular pathways. One of the most successful novel approaches in the treatment of ACC involves therapeutic agents that inhibit the neovascularization process of growing tumors [25]. Bevacizumab is a recombinant humanized anti-vascular endothelial growth factor monoclonal antibody that is being clinically evaluated in many tumor types, including ACC. Because bevacizumab was only recently made available in Korea as first-line chemotherapy, only 29 patients received bevacizumab.
Conclusion
This study confirms that both oxaliplatin- and irinotecan-containing combination chemotherapy are effective for the first-line treatment of ACC. Capecitabine clearly represents an effective and well-tolerated oral alternative to 5-FU. While the current study was primarily focused on cytotoxic therapies, the integration of targeted agents, including bevacizumab, is a novel standard option to further improve outcomes for patients with ACC.
Acknowledgments
The present research was conducted by the research fund of Dankook University (Cheonan, Korea) in 2009.
Notes
Conflict of interest relevant to this article was not reported.