AbstractPurposeFeatures of epidermal growth factor receptor (EGFR) expression in osteosarcoma and in vitro efficacies of EGFR inhibitors against osteosarcoma cells were evaluated.
Materials and MethodsThirty biopsy samples of osteosarcoma patients were retrospectively analyzed for EGFR protein expression by immunohistochemistry. Relationships between EGFR expression and clinicopathologic characteristics and treatment outcomes were evaluated. Four osteosarcoma cell lines were analyzed for EGFR and p-EGFR expression by western blotting. Efficacies of gefitinib and BIBW2992 on osteosarcoma cells were evaluated using a 3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide assay. Tyrosine kinase domains in exons 18 to 21 were sequenced and gene expression analyses of EGFR and PTEN were performed in four osteosarcoma cell lines.
ResultsEGFR protein was expressed in 27 (90%) samples (6 low, 12 intermediate, 9 high) and in three cell lines. Intermediate or high staining for EGFR was related to a tumor volume<150 mL (p<0.001) and histologic subtype other than osteoblastic type (p=0.03). However, EGFR expression was not associated with histologic response to preoperative chemotherapy or survival. Gefitinib and BIBW 2992 did not have any significant inhibitory effect on cell viabilities. DNA sequencing analysis revealed three osteosarcoma cell lines have single base changes at codon 2361 of exon 20 (G to A), without affecting translation results. Furthermore, no mutation was found to be associated with constitutive EGFR activation.
IntroductionIntroduction of multiagent chemotherapy has resulted in significantly improved survival of patients with osteosarcoma [1,2]. However, improvements in survival have reached a plateau [3], and treatment outcomes for patients with metastasis or relapsed disease remain dismal [4-6]. Thus, novel agents that act via different mechanisms are needed in order to achieve further improvement in the survival rate [2,6].
Recent advances in molecular biology have resulted in identification of several pathways involved in the pathogenesis and progression of cancer. One of these is the epidermal growth factor receptor (EGFR) pathway, which is believed to be involved in progression of lung, colon, head, and neck cancers [7-10]. Following the success of gefitinib for treatment of non-small cell lung cancer [7,8], agents targeting EGFR via different mechanisms have been developed; some of these are currently undergoing clinical trials for treatment of colon, head, and neck cancers [10,11].
Although a large number of studies have been conducted for characterization of expression of growth factor receptors in bone and soft tissue tumors [12-14], the roles played by EGFR family members in osteosarcoma remain elusive. In vitro studies have reported expression of EGFR in osteosarcoma cells as well as effective inhibition of growth of osteosarcoma cells by EGFR inhibitors [15-17]. Expression of EGFR has been reported in 40-81% of osteosarcoma tumor tissues [13,14,17], however, its association with prognosis has been controversial. In one study, expression of EGFR showed an association with shorter overall survival (OS) of patients with osteosarcoma [17], while others have reported an association of its expression with good clinical outcome [18]. Furthermore, most of these studies analyzed Euro-American cases, and data on expression of EGFR in Asian patients with osteosarcoma is rare.
In the present study, we conducted a retrospective analysis of EGFR protein expression in osteosarcoma tumor samples obtained from Korean patients and examined associations between its expression and clinical features and treatment outcomes. In addition, in vitro studies were performed for evaluation of the efficacy of EGFR inhibitors, gefitinib and BIBW2992, on proliferation of osteosarcoma cells.
Materials and Methods1. Patients and treatmentThirty patients with primary osteosarcoma, treated at the Korea Cancer Center Hospital between 1995 and 2007 were retrospectively analyzed. The study was approved by the Institutional Review Board of Korea Cancer Center Hospital. Patients met the following criteria: 1) high-grade osteosarcoma; 2) no distant metastasis at the time of diagnosis; 3) no history of previous treatment; and 4) the availability of an incisional biopsy specimen taken prior to chemotherapy. A detailed summary of patient information is shown in Table 1. Treatments were dependent on concurrent medical problems. Two patients (case numbers 29 and 30) underwent surgery only, whereas the remaining 28 patients underwent two courses of preoperative chemotherapy followed by four courses of postoperative chemotherapy. Details regarding treatment have been previously described [19].
2. Immunohistochemical stainingRepresentative areas, without spontaneous necrosis, were selected from incisional biopsy samples. We used a Zymed nonbiotin amplification system (Zymed Laboratories, South San Francisco, CA). Primary goat anti-human EGFR polyclonal anti-body and anti-goat EGFR biotinylated secondary antibody were purchased from Santa Cruz Biotechnology (Santa Cruz, CA). EGFR immunoreactivity was observed in membranes or cytoplasm of osteosarcoma cells. Some tissues showed strong immunoreactivity for EGFR, whereas others showed moderate or no immunoreactivity. Staining intensity was interpreted as follows: low, positivity of <10% of tumor cells; intermediate, positivity of 10-50% of tumor cells; and high, positivity of >50% of tumor cells.
3. Cell proliferation assaysHuman osteosarcoma cell lines HOS, KHOS/NP, MG-63, and U-2 OS were obtained from the American Type Culture Collection (ATCC; Manassas, VA). Gefitinib and BIBW2992 were purchased from SelleckChem (S1025, S1011, Houston, TX), dissolved in dimethyl sulfoxide, and stored at -20℃. In each well of 96-well plates, 5,000 cells in 50 µL of media were seeded and incubated overnight at 37℃ in a humidified 5% CO2 incubator. On the following day, gefitinib and BIBW 2992 (0.01-20 µM) were added to wells and plates, followed by incubation for an additional 72 hours. A 3-(4, 5-dimethylthiazol-2-yl)-2, 5-diphenyltetrazolium bromide (MTT) assay was used for measurement of cell proliferation. IC50 values were determined from dose-response curves.
4. Western blot analysisCell lysates were prepared using a kit from Cell Signaling Technology (Beverly, MA). Equal amounts of protein (determined using the Bio-Rad Protein assay, Bio-Rad, Hercules, CA) were run on 12% sodium dodecyl sulfate polyacrylamide gel electrophoresis gels and transferred to polyvinylidene fluoride membranes, which were washed with Tris-buffered saline (TBS) containing 0.1% Tween 20 (TTBS), blocked with TTBS and 5% wt/vol nonfat dry milk overnight at 4℃, and incubated with primary antibody at 1 : 1,000 dilution. Membranes were then washed with TTBS, followed by incubation with horseradish peroxidase-conjugated secondary antibody (1 : 1,000). Signals were detected using an Amersham ECL (GE Healthcare Life Sciences, Munich, Germany).
5. EGFR mutation analysisThe genomic DNAs of the four osteosarcoma cell lines were extracted using a High Pure PCR template Preparation kit (Roche, Mannheim, Germany). PCR and real-time amplification monitoring of peptide nucleic acid PCR clamping were performed using a CFX 96 system (Bio-Rad). Genomic PCR was performed in final volume DNA and 0.75 U Taq polymerase (Solgent, Daejeon, Korea). The following sequencing primers were employed: E18-SF, 5-AGGTGACCCTTGTCTCTGTG-3, E18-SR, and 5-CCTGTGCCAGGGACCTTAC-3 for exon 18; E19-SF, 5-CATGTGGCACCATCTCACAA-3, E19-SR, and 5-CCCACA CAGCAAAGCAGAA-3 for exon 19; E20-B-F, 5-ATCGCATTCATGCGTCTTC-3, E20-B-R, and 5-GTCTTTGTGTTCCCGGACAT-3 for exon 20; E21-B-F, 5-CCTCACAGCAGGGTCTTCTC-3, E21-BR, and 5-GGAAAATGCTGGCTGACCTA-3 for exon 21. Sequences were compared with the GenBank-archived sequence of human EGFR.
6. Gene expression analysisA Low Input Quick Amp labeling kit (Agilent Technologies, Santa Clara, CA) was used for labeling and amplification of total RNA samples (200 ηg), and Cy3-labeled amplified RNAs (aRNA) were re-suspended in 50 µL of hybridization solution (Agilent Technologies). Labeled aRNAs were then placed on an Agilent SurePrint G3 Human GE 8×60K array (Agilent Technologies) and covered with a Gasket 8-plex slide (Agilent Technologies). The slides were hybridized for 17 hours at 65℃, washed in 2× saline sodium citrate (SSC) containing 0.1% sodium dodecyl sulfate for 2 minutes, 1×SSC for 3 minutes, and then in 0.2×SSC for 2 minutes at room temperature, followed by centrifugation at 1,800× g for 20 seconds for drying. An Agilent scanner and its on-board software were used for analysis of arrays. Feature Extraction v10.7.3.1 (Agilent Technologies) was used for calculation of gene expression levels, and the Robust Multi-Array Average algorithm was used for generation of relative signal intensities for each gene. The quantile normalization method in GeneSpring GX 11.5.1 (Agilent Technologies) was used for processing of data.
7. Statistical analysisThe chi-square test was used for analysis of correlations between categorical clinicopathologic variables and EGFR expression. Variables analyzed included age, sex, tumor location, histologic subtype, tumor volume, and histologic response to preoperative chemotherapy. Tumor volumes were calculated using the ellipsoid formula [V = (4π/3)abc, where a, b, and c represent length, width, and depth] [19]. Kaplan-Meier survival analysis was used to examine relations between clinicopathologic variables and events (defined as either local recurrence, metastasis, or death). The log-rank test was used for calculation of survival differences according to clinicopathologic variables. SPSS ver. 11.5 (SPSS Inc., Chicago, IL) was used in performance of all calculations, and p-values of <0.05 were considered significant.
Results1. EGFR protein expression, clinicopathologic characteristics, and outcomeTwenty-seven (90.0%) biopsy samples showed positive staining for EGFR protein (Table 1, Fig. 1); staining intensities for EGFR protein were as follows: high in 9, intermediate in 12, and low in 6. Neither the presence of EGFR staining nor its intensity showed an association with age, sex, tumor location, or histologic response to preoperative chemotherapy (Table 2). However, intermediate or high staining intensity for EGFR was related to a smaller tumor volume (p<0.001) and a histologic subtype other than osteoblastic type (p=0.03).
In addition, EGFR positivity and its staining intensity did not appear to be related to the survival (Fig. 2). Five-year OS for our 30 patients was 49.2±9.3%. Patients were followed for a median of 40.4 months (range, 6.0 to 126.0 months), and there were 17 events (14 distant metastases, 1 local recurrence, and 2 local recurrences combined with distant metastasis). Metastatic sites were as follows: lung (n=9), bone (n=3), lung and bone (n=3), adrenal gland (n=1), and pancreas (n=1). Median event-free survival for the 17 patients who experienced an adverse event was 9.3 months (range, 2.0 to 40.4 months).
2. Effect of EGFR inhibitors on the viabilities of osteosarcoma cell linesFor the four osteosarcoma cell lines tested, expression of EGFR protein was observed in HOS, MG-63, and KHOS/NP cells, however, expression of p-EGFR was not observed in any cell line under basal culture conditions (Fig. 3). Osteosarcoma cells were exposed to gefitinib or BIBW2992 at concentrations ranging from 0 to 20 µM for 72 hours. However, no dose-dependent inhibitory effect was observed in any of the cell lines (Fig. 4).
3. Gene expression and mutation analysis of osteosarcoma cell lines
Table 3 shows expression of EGFR and phosphatase and tensin homolog (PTEN) in osteosarcoma cell lines. Expression of EGFR was observed at higher levels and its level of expression showed concurrence with western blot findings. However, PTEN was expressed at lower levels.
In the meantime, the tyrosine kinase domain from exons 18 to 21 was sequenced in all four cell lines, in order to determine whether they harbor constitutively activating mutations that confer sensitivity to tyrosine kinase inhibitors. We found single base changes at codon 2361 in exon 20 in HOS, MG-63, and KHOS/NP cells (G to A). However, these changes did not result in amino acid changes. Furthermore, we failed to find any known mutation associated with constitutive activation of EGFR in any of the four cell lines.
DiscussionIn the present study, we found that EGFR protein is frequently expressed in osteosarcoma biopsy samples and cell lines. However, we found no association between expression of EGFR protein and treatment outcome, and, in addition, EGFR inhibitors gefitinib and BIBW2992 had no significant inhibitory effect on the viabilities of osteosarcoma cells. A single nucleotide change in the EGFR tyrosine kinase domain was identified by mutation analysis in all four osteosarcoma cell lines examined, however, no activating mutation was found.
Some limitations of the present study must be considered. First, due to the retrospective nature of this study, our study cohort included only a small number of patients who were treated over two decades. Thus, patients were not prospectively randomized and treatments were heterogeneous. Second, we believe that selection bias must have existed; for example, inclusion of patients who are older than 40 years. And the poor survival might have masked the prognostic significance of EGFR expression. Third, the reliance on immunohistochemistry and semiquantitative measures used for assessment of EGFR expression imposes limitations. Forth, although EGFR mutation status should have been determined in biopsy samples, due to the small sample sizes, it was limited to the four cell lines.
Relations between EGFR expression and the clinicopathologic characteristics of osteosarcoma remain elusive. In previous studies, involvement of EGFR in progression of lung, colon, head, and neck cancers has been suggested [7-11,20]. Thus, we supposed that EGFR expression might be related to the aggressive characteristics and poor treatment outcome of osteosarcoma. However, we found no relation between EGFR expression and treatment outcome; actually, an association with a small tumor volume was observed, which was not expected. We believe that this finding was probably due to the small sample size and section bias, however, it may be that the role of EGFR in osteosarcoma differs from that in adult carcinomas. Little data are available on the association between EGFR expression and clinical outcome in osteosarcoma. Freeman et al. [16] also failed to detect any association between EGFR expression and clinical findings in osteosarcoma, however, Kersting et al. [18] concluded that EGFR expression has a dose-dependent association with better prognosis in patients with high-grade osteosarcoma. Conduct of additional studies to elucidate the mechanism responsible for EGFR expression and for the clinicopathologic characteristics of osteosarcoma will be needed.
Contrary to our expectation, we observed no inhibitory effect of gefitinib and BIBW2992 on the viabilities of osteosarcoma cells. In order for EGFR-directed therapy to be available in osteosarcoma, assessment of its activation status and impact of its signaling on cell proliferation as well as the relationship between its expression and outcome need to be clarified. It has previously been suggested that osteosarcoma might be biologically dependent on EGFR-modulated cell signaling pathways [12,13,15,21,22]. Although expression of EGFR protein was observed in the four osteosarcoma cell lines that we tested, none of them expressed p-EGFR. It has been suggested that neither the expression level nor the phosphorylation status of EGFR showed correlation with sensitivity to gefitinib [23]. Although we tested gefitinib and BIBW2992 at different concentrations, we failed to observe any significant inhibitory effect on cell viability. The mutational status of EGFR has been reported to modulate responsiveness to EGFR inhibitors [9,24], therefore, we analyzed the tyrosine kinase domain of EGFR in the four osteosarcoma cell lines. Although an EGFR polymorphism was found in exon 20, it did not result in an amino acid change. In addition, we did not identify any activating mutation known to confer susceptibility to EGFR inhibitors. The osteosarcoma cell lines used in the present study exhibited slightly lower PTEN expression, loss of which is associated with resistance to anti-EGFR tyrosine kinase inhibitors [9,24]. The possibility exists that the lack of EGFR mutation and efficacy of EGFR inhibitors might be related to the cells we used. The cell lines analyzed were not of early passages, but were of multiple passages that might have accumulated many changes that were not present in the primary tumor specimens. Or, other EGFR-directed treatment modalities might be effective in osteosarcoma. Recently it was reported that anti-EGFR antibody cetuximab enhances the cytolytic activity of natural killer cell toward osteosarcoma cells [25]. Available data suggest the probable existence of subtle interplay between different growth factor receptors and downstream molecules in osteosarcoma. Conduct of further studies to elucidate the roles of EGFR and its inhibitors in osteosarcoma will be needed.
ConclusionWe found that EGFR protein is frequently expressed in osteosarcoma, however, this expression showed no association with treatment outcome. In addition, the two EGFR inhibitors, gefitinib and BIBW2992, had no observable inhibitory effect on viability of osteosarcoma cells, and mutation analysis of the EGFR tyrosine kinase domain failed to identify any activating mutation. However, considering that our study was performed using a limited number of biopsy samples and cell lines, and evaluated two kinds of EGFR inhibitors, conduct of further studies to explore the potential of other therapeutic agents targeting EGFR will be necessary.
AcknowledgmentsThis study was supported by the Clinical Radiological Research Project, Korea Institute of Radiological and Medical Sciences (Grant No. 50459-2010).
References1. Bacci G, Longhi A, Fagioli F, Briccoli A, Versari M, Picci P. Adjuvant and neoadjuvant chemotherapy for osteosarcoma of the extremities: 27 year experience at Rizzoli Institute, Italy. Eur J Cancer. 2005;41:2836–2845. PMID: 16298125
2. Gorlick R, Anderson P, Andrulis I, Arndt C, Beardsley GP, Bernstein M, et al. Biology of childhood osteogenic sarcoma and potential targets for therapeutic development: meeting summary. Clin Cancer Res. 2003;9:5442–5453. PMID: 14654523
3. Bacci G, Forni C, Ferrari S, Longhi A, Bertoni F, Mercuri M, et al. Neoadjuvant chemotherapy for osteosarcoma of the extremity: intensification of preoperative treatment does not increase the rate of good histologic response to the primary tumor or improve the final outcome. J Pediatr Hematol Oncol. 2003;25:845–853. PMID: 14608193
4. Eselgrim M, Grunert H, Kuhne T, Zoubek A, Kevric M, Burger H, et al. Dose intensity of chemotherapy for osteosarcoma and outcome in the Cooperative Osteosarcoma Study Group (COSS) trials. Pediatr Blood Cancer. 2006;47:42–50. PMID: 16206218
5. Kager L, Zoubek A, Potschger U, Kastner U, Flege S, Kempf-Bielack B, et al. Primary metastatic osteosarcoma: presentation and outcome of patients treated on neoadjuvant Cooperative Osteosarcoma Study Group protocols. J Clin Oncol. 2003;21:2011–2018. PMID: 12743156
6. Meyers PA, Gorlick R, Heller G, Casper E, Lane J, Huvos AG, et al. Intensification of preoperative chemotherapy for osteogenic sarcoma: results of the Memorial Sloan-Kettering (T12) protocol. J Clin Oncol. 1998;16:2452–2458. PMID: 9667263
7. Herbst RS, Kies MS. ZD1839 (Iressa) in non-small cell lung cancer. Oncologist. 2002;7(Suppl 4):9–15. PMID: 12202783
8. Raben D, Helfrich BA, Chan D, Johnson G, Bunn PA Jr. ZD1839, a selective epidermal growth factor receptor tyrosine kinase inhibitor, alone and in combination with radiation and chemotherapy as a new therapeutic strategy in non-small cell lung cancer. Semin Oncol. 2002;29(1 Suppl 4):37–46. PMID: 11894012
9. Vivanco I, Mellinghoff IK. Epidermal growth factor receptor inhibitors in oncology. Curr Opin Oncol. 2010;22:573–578. PMID: 20739887
10. Yarom N, Jonker DJ. The role of the epidermal growth factor receptor in the mechanism and treatment of colorectal cancer. Discov Med. 2011;11:95–105. PMID: 21356164
11. Sharafinski ME, Ferris RL, Ferrone S, Grandis JR. Epidermal growth factor receptor targeted therapy of squamous cell carcinoma of the head and neck. Head Neck. 2010;32:1412–1421. PMID: 20848399
12. Dobashi Y, Suzuki S, Sugawara H, Ooi A. Involvement of epidermal growth factor receptor and downstream molecules in bone and soft tissue tumors. Hum Pathol. 2007;38:914–925. PMID: 17376509
13. Dobashi Y, Takei N, Suzuki S, Yoneyama H, Hanawa M, Ooi A. Aberration of epidermal growth factor receptor expression in bone and soft-tissue tumors: protein overexpression, gene amplification and activation of downstream molecules. Mod Pathol. 2004;17:1497–1505. PMID: 15254554
14. Oda Y, Wehrmann B, Radig K, Walter H, Rose I, Neumann W, et al. Expression of growth factors and their receptors in human osteosarcomas Immunohistochemical detection of epidermal growth factor, platelet-derived growth factor and their receptors: its correlation with proliferating activities and p53 expression. Gen Diagn Pathol. 1995;141:97–103. PMID: 8548600
15. Do SI, Jung WW, Kim HS, Park YK. The expression of epidermal growth factor receptor and its downstream signaling molecules in osteosarcoma. Int J Oncol. 2009;34:797–803. PMID: 19212684
16. Freeman SS, Allen SW, Ganti R, Wu J, Ma J, Su X, et al. Copy number gains in EGFR and copy number losses in PTEN are common events in osteosarcoma tumors. Cancer. 2008;113:1453–1461. PMID: 18704985
17. Wen YH, Koeppen H, Garcia R, Chiriboga L, Tarlow BD, Peters BA, et al. Epidermal growth factor receptor in osteosarcoma: expression and mutational analysis. Hum Pathol. 2007;38:1184–1191. PMID: 17509661
18. Kersting C, Gebert C, Agelopoulos K, Schmidt H, van Diest PJ, Juergens H, et al. Epidermal growth factor receptor expression in high-grade osteosarcomas is associated with a good clinical outcome. Clin Cancer Res. 2007;13:2998–3005. PMID: 17505002
19. Lee JA, Kim MS, Kim DH, Lim JS, Yoo JY, Koh JS, et al. Relative tumor burden predicts metastasis-free survival in pediatric osteosarcoma. Pediatr Blood Cancer. 2008;50:195–200. PMID: 18061933
20. Batus M, Fidler MJ, Bonomi PD. Primary and secondary therapeutic strategies for EGF receptor pathway inhibition in non-small-cell lung cancer. Expert Rev Anticancer Ther. 2010;10:1589–1599. PMID: 20942630
21. Hughes DP, Thomas DG, Giordano TJ, McDonagh KT, Baker LH. Essential erbB family phosphorylation in osteosarcoma as a target for CI-1033 inhibition. Pediatr Blood Cancer. 2006;46:614–623. PMID: 16007579
22. Stewart CF, Leggas M, Schuetz JD, Panetta JC, Cheshire PJ, Peterson J, et al. Gefitinib enhances the antitumor activity and oral bioavailability of irinotecan in mice. Cancer Res. 2004;64:7491–7499. PMID: 15492275
23. Sirotnak FM, Zakowski MF, Miller VA, Scher HI, Kris MG. Efficacy of cytotoxic agents against human tumor xenografts is markedly enhanced by coadministration of ZD1839 (Iressa), an inhibitor of EGFR tyrosine kinase. Clin Cancer Res. 2000;6:4885–4892. PMID: 11156248
24. Mellinghoff IK, Wang MY, Vivanco I, Haas-Kogan DA, Zhu S, Dia EQ, et al. Molecular determinants of the response of glioblastomas to EGFR kinase inhibitors. N Engl J Med. 2005;353:2012–2024. PMID: 16282176
25. Pahl JH, Ruslan SE, Buddingh EP, Santos SJ, Szuhai K, Serra M, et al. Anti-EGFR antibody cetuximab enhances the cytolytic activity of natural killer cells toward osteosarcoma. Clin Cancer Res. 2012;18:432–441. PMID: 22090361
Fig. 1Immunohistochemical staining for epidermal growth factor receptor protein in initial biopsy samples from patients with osteosarcoma. (A) Negative. (B) Low. (C) Intermediate. (D) High (A-D, ×400). 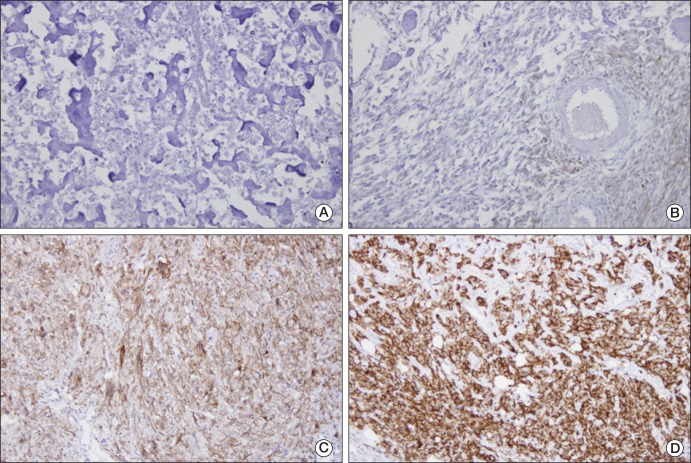
Fig. 2Epidermal growth factor receptor protein expression and survival of patients with localized osteosarcoma. 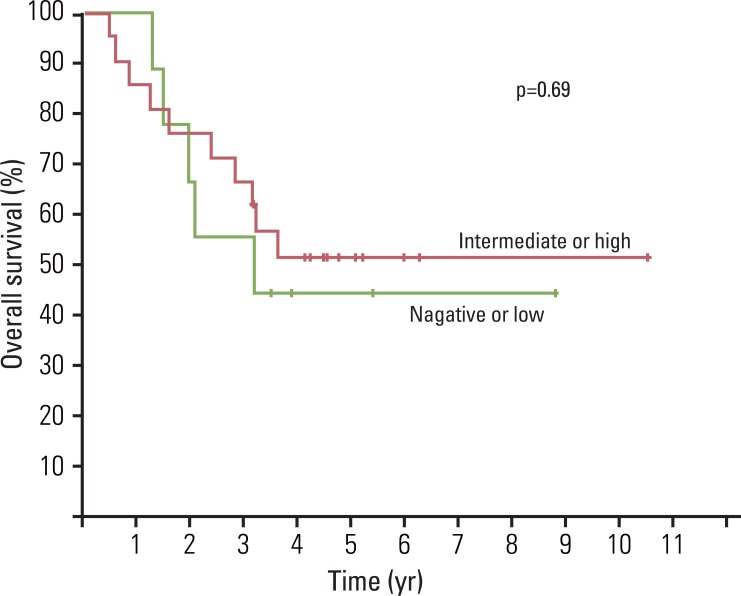
Fig. 3Epidermal growth factor receptor (EGFR) and p-EGFR expression of osteosarcoma cell lines in basal culture conditions. 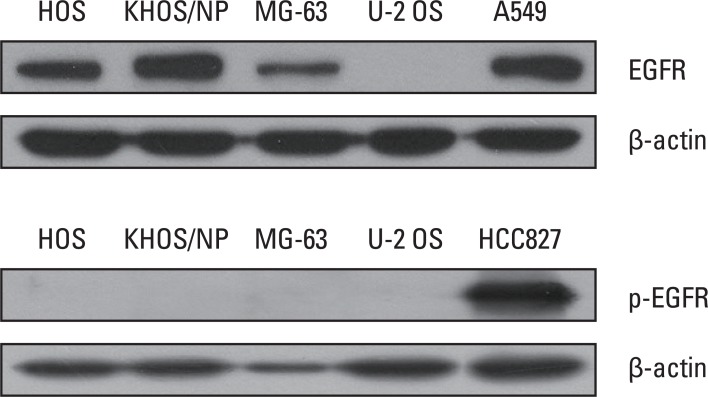
Table 1Patients' Characteristics Table 2Clinicopathologic variables and EGFR protein expression Table 3Up- or down-regulation of genes in osteosarcoma cells vs. universal human reference RNA |
|
|||||||||||||||||||||||||||||||||||||