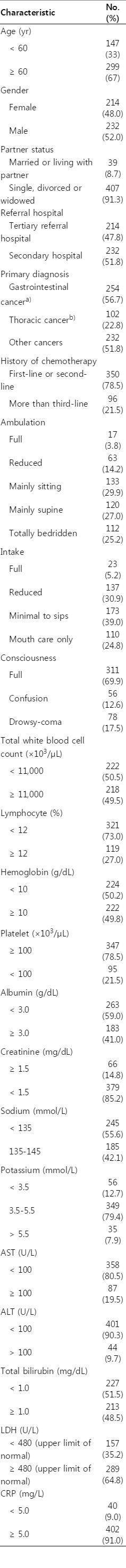Patient’s Factors at Entering Hospice Affecting Length of Survival in a Hospice Center
Article information
Abstract
Purpose
In order to provide effective hospice care, adequate length of survival (LOS) in hospice is necessary. However the reported average LOS is much shorter. Analysis of LOS in hospice has not been reported from Korea. We evaluated the duration of LOS and the factors associated with LOS at our hospice center.
Materials and Methods
We retrospectively examined 446 patients who were admitted to our hospice unit between January 2010 and December 2012. We performed univariate and multivariate analysis for analysis of factors associated with LOS.
Results
The median LOS was 9.5 days (range, 1 to 186 days). The LOS of 389 patients (86.8%) was< 1 month. At the time of admission to hospice, 112 patients (25.2%) were completely bedridden, 110 patients (24.8%) had mouth care only without intake, and 134 patients (30.1%) had decreased consciousness, from confusion to coma. The median time interval between the day of the last anticancer treatment and the day of hospice admission was 75 days. By analysis of the results of multivariate analysis, decreased intake and laboratory results showing increased total white blood cell (WBC), decreased platelet count, increased serum creatinine, increased aspartate aminotransferase (AST), alanine aminotransferase (ALT), and lactate dehydrogenase (LDH) level were poor prognostic factors for survival in hospice.
Conclusion
Before hospice admission, careful evaluation of the patient’s performance, particularly the oral intake, and total WBC, platelet, creatinine, AST, ALT, and LDH level is essential, because these were strong predictors of shorter LOS. In the future, conduct of prospective controlled studies is warranted in order to confirm the relationship between potential prognostic factors and LOS in hospice.
Introduction
End of life care in hospice is expanding globally. For effective hospice care, adequate length of survival (LOS) in hospice is necessary. To improve the LOS in hospice, it is essential that physicians refer patients at the appropriate time, and the hospice team must select the indicated patients for hospice care from the referred patients. If the LOS of the hospice patient is too short, they do not receive adequate help from hospice and their short LOS can have a negative impact on other patients who share the same ward. Therefore, another type of palliative care, such as home hospice care is required for these patients.
Despite some previous reports, there are no established criteria for selection of patients who are more likely to live longer in hospice. Many physicians had a tendency to overestimate the LOS of terminal cancer patients [1,2]. According to previous studies, there was a considerable physician factor for LOS in hospice; LOS was adequate when the referring physician had previously referred more than two patients to hospice care and estimated patient survival accurately [3]. In addition, social factors, local market factors, and accessibility to medical institutions showed an association with early referral to hospice care [4]. Significant differences in LOS were observed according to gender, diagnosis, physician specialty, referral source, type of insurance, living status, and discharge status [5]. In a recent study, factors showing association with adequate LOS were full-code status, receiving hospice care at home, hospitalization during enrollment in hospice, referral to hospice by an oncologist, and a diagnosis of cancer [6].
In this country, no previous study on LOS in hospice and affecting factors has been reported. Therefore, we evaluated the current length of hospice stay and analyzed the patient’s factors regarding enrolled time that influenced LOS in hospice.
Materials and Methods
1. Patients
We retrospectively examined 446 patients who were admitted to Bucheon St. Mary’s Hospital between January 1, 2010, and December 31, 2012. We studied baseline characteristics of these patients. The patients were classified according to age (< 60, ≥ 60), sex (male, female), partner status (married, or living with a partner; or single, divorced, or widowed), referral hospital (secondary, tertiary), primary diagnosis (gastrointestinal cancer, thoracic cancer, or other cancers), history of chemotherapy (first-line to second-line, more than third-line), ambulation (full, reduced, mainly sitting, mainly supine, totally bedridden), intake (full, reduced, minimal to sips, mouth care only), and consciousness (full, confusion, drowsy to coma). We tried to find the important laboratory results as a prognostic factor. We performed laboratory studies for patients entering hospice. The patients were classified according to the total white blood cell (WBC) count (< 11,000×103/μL, ≥ 11,000×103/μL), lymphocyte percentage (< 12%, ≥ 12%), hemoglobin (< 10 g/dL, ≥ 10 g/dL), platelet (< 100×103/μL, ≥ 100×103/μL), albumin (< 3.0 g/dL, ≥ 3.0 g/dL), creatinine (< 1.5 mg/dL, ≥ 1.5 mg/dL), sodium (< 135 mmol/L, 135 to 145 mmol/L, > 145 mmol/L), potassium (< 3.5 mmol/L, 3.5 to 5.5 mmol/L, > 5.5 mmol/L), aspa-rtate aminotransferase (AST; < 100 U/L, ≥ 100 U/L), alanine aminotransferase (ALT; < 100 U/L, ≥ 100 U/L), total bilirubin (< 1.0 mg/dL, ≥ 1.0 mg/dL), lactate dehydrogenase (LDH; < 480, ≥ 480), and C-reactive protein (CRP; < 5.0 mg/L, ≥ 5.0 mg/L). LOS was the time interval between the day of admission to hospice and the day of the patient’s death.
2. Statistical methods
The median LOS in hospice and the median referral time to hospice were calculated. Using the Kaplan-Meier method, we analyzed the association between LOS and the patients’ baseline demographics (age, sex, marital status, referral hospital, types of cancer, history of chemotherapy), palliative performances (ambulation, intake, consciousness), and laboratory findings (total WBC count, lymphocyte percentage, hemoglobin, platelet, albumin, creatinine, sodium, potassium, AST, ALT, total bilirubin, LDH, CRP). Factors showing significant association with LOS by univariate analysis were evaluated by multivariate analysis using Cox proportional-hazards regression for identification of factors showing independent association with LOS. Analysis was performed using the SPSS ver. 20.0 software package (SPSS Inc., Chicago, IL).
Results
1. Baseline characteristics of patients
The median age of the hospice patients was 66 years (range, 13 to 94 years). The baseline demographics of the patients treated at our hospice center are shown in Table 1; 299 patients (67%) were > 60 years old, 232 patients (52%) were male; 407 patients (91.3%) were not living with their spouse or a partner (they were single, divorced, or widowed); 214 patients (47.8%) were referred by a tertiary hospital; and 232 patients (51.8%) were referred by a secondary hospital. The primary diagnosis was gastrointestinal cancer in 254 patients (56.7%), thoracic cancer in 102 patients (22.8%), and other cancers in 90 patients (20.1%). Three hundred fifty patients (78.5%) had previously received first-line to second-line chemotherapy before and 96 patients (21.5%) had received more than third-line chemotherapy. At the time of admission to hospice, 112 patients (25.2%) were completely bedridden, 110 patients (24.8%) had mouth care only without intake, and 134 patients (30.1%) had decreased consciousness such as confusion or drowsy to coma. The classifications of the patients according to laboratory results are shown in Table 1. All patients agreed to an informed consent for ‘do not resuscitate’ (DNR).
2. Referral time to hospice and LOS in hospice
The median time interval between diagnosis of stage IV or recurrent cancer and referral to hospice was 248 days (range, 1 to 4,405 days). The median time interval between the last day of anticancer treatment and the day of hospice admission was 75 days (range, 3 to 1,310 days). The median LOS was 9.5 days (range, 1 to 186 days) (Table 2). The LOS of 389 patients (86.8%) was less than one month.
3. Factors affecting LOS in hospice
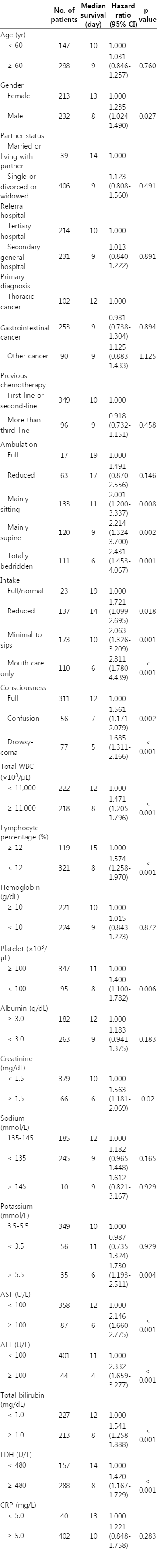
In univariate analysis, factors showing significant association with LOS included sex (p=0.027), intake (p < 0.02), consciousness (p < 0.01), total WBC (p < 0.001), lymphocyte percentage (p < 0.001), platelet (p=0.006), creatinine (p=0.02), potassium (p=0.004), AST (p < 0.001), ALT (p < 0.001), total bilirubin (p < 0.001), and LDH (p < 0.001) (Table 3). In ambulation status, no statistical significance was observed between ‘full’ and ‘reduced’ (p=0.146). Age, partner status, referral hospital, primary diagnosis, history of chemotherapy, hemoglobin, albumin, sodium, potassium, and CRP level did not show a statistically significant result.
In multivariate analysis, factors showing significant association with LOS, included intake (p < 0.05), total WBC (p<0.001), platelet (p=0.015), creatinine (p=0.007), AST (p=0.03), ALT (p=0.008), and LDH (p=0.006) (Table 4). As the intake status becomes gradually worse to reduced, minimal to sips, mouth care only, the hazard ratio of short LOS in hospice was increased (hazard ratio, 1.525, 2.096, 2.732). In multivariate analysis, sex, consciousness, lymphocyte percentage, potassium, and total bilirubin did not show a statistically significant result.
Discussion
End of life care for terminal cancer patients is very important and terminal care in hospice is becoming universal. Although LOS in hospice does not show exact correlation with the quality of care, LOS has an important influence on the effect of hospice treatment. There is general agreement among experts in the field and referring clinicians that patients who are referred near the end of life receive fewer benefits from the services that hospice offers. Thus, there is a widespread consensus among experts, referring clinicians, and government agencies that many patients should be enrolled in hospice sooner [7-10]. Because there was little information on LOS in hospice and the factors affecting LOS in South Korea, we conducted this study.
At the time of admission to hospice, 112 patients (25%) were completely bedridden, corresponding to below 30% of the Palliative Performance Scale (PPS) ver. 2. Similarly, 110 patients (24.6%) had mouth care only without intake, below 10% of the PPS. In addition, 134 patients (30.6%) had decreased consciousness from confusion to coma, below 10% of the PPS. These results indicate that the palliative performance of these patients was poorer than reported from previous studies of hospices from other countries [11,12].
Compared with other studies, we found a relatively longer time period (median, 75 days) from the last anticancer treatment to referral to hospice. In addition, the median LOS in hospice was 9.5 days (range, 1 to 186 days), significantly shorter than that reported in another study [13]. Reasons for the late referrals could be multiline chemotherapy and longer duration of anticancer treatment. In addition, insufficient in-advance discussion about preferred end of life care between patients/families and physicians or families’ insufficient preparation for changes of patient conditions could be important reasons for late referral, as found in a previous study [14]. In this study, 96 patients (21.5%) underwent more than third-line chemotherapy before referral to our hospice. Considering that third-line palliative chemotherapy has no established survival benefit in most cancer patients, further treatment should be avoided, therefore, early hospice referral was appropriate for most of the patients.
In this study, in univariate analysis, male sex (p=0.027), less intake (p < 0.02), and lower consciousness (p < 0.005) showed an association with shorter LOS in hospice. These findings were consistent with those of previous studies [15-17]. Although previous studies showed that the performance status was an important factor, our study analyzed the detail factors of performance status; according to the result, intake status and consciousness were more significant factors than ambulation. Regarding laboratory results as a prognostic factor, previous studies showed that total WBC count, lymphocyte percentage, and bilirubin were significant factors [18,19]. In our study, these factors were also statistically significant, and platelet count, serum creatinine, potassium, AST, ALT and LDH were additional significant factors affecting LOS in hospice.
In analysis of the results of multivariate analysis, intake, total WBC, platelet, creatinine, AST, ALT, and LDH were significant factors, indicating that intake status is the most important prognostic factor of performance factors. Regarding the laboratory findings, increased total WBC, decreased platelet count, increased serum creatinine, AST, ALT and increased LDH level were poor prognostic factors for survival in hospice. Increased total WBC count is related to infection or leukemoid reaction, decreased platelet count is related to sepsis or disseminated intravascular coagulopathy (DIC). Increased serum creatinine and AST, ALT level is related to decreased renal and hepatic function. Elevated LDH level is usually an indicator of high tumor burden, although it is not directly proportional to the tumor burden. All of these laboratory results are related to cancer progression and decreased overall physical function of the patient. Therefore, we strongly recommend careful evaluation of the patients’ oral intake status and total WBC, platelet from complete blood count, and serum creatinine, AST, ALT, and LDH level from blood chemistry at the time of referral to hospice.
This study had some limitations. First, this study was a single center study. For greater external validity, a multicenter study is necessary. Second, because we retrospectively studied baseline characteristics we could not analyze the activity and self-care components of the PPS. In the future, conduct of a prospective controlled study is warranted in order to study palliative performance with greater detail. Third, LOS of hospice is not the sole factor influencing quality in hospice care. According to some studies, it is important for patients and their family members to be satisfied with not just the LOS in hospice but also the quality of hospice care [20-22]. Therefore, conduct of further research is warranted with regard to both lengthening LOS in hospice and for improving the satisfaction of patients and their families despite a short LOS in hospice.
Conclusion
The LOS of hospice in our institution was too short relative to recommendations and other studies. It appears that illness progressed during the relatively long delay between diagnosis of incurable cancer and referral to hospice; consequently, by the time patients were referred to hospice their performance was poor and their overall physical function was decreased due to progression of cancer, which could have negatively affected LOS in hospice. Before hospice admission, careful evaluation of the oral intake and total WBC, platelet, creatinine, AST, ALT, and LDH level is essential because these were strong predictors of shorter LOS. In the future, we should conduct a prospective study of the subjective symptoms of patients entering hospice on affecting LOS as well as the above objective factors of the patient. In addition, investigation of the appropriate LOS in hospice for satisfaction of patients and their family members in this country is also needed.
Notes
Conflict of interest relevant to this article was not reported.